The Truth About Birth Control Pills: What Medical Experts Want You to Know

Introduction
More than 85 % of post‑menopausal women report at least one bothersome symptom, and up to 40‑50 million women in the United States experience vasomotor complaints such as hot flashes. Because menopause is a natural life stage, many seek relief without immediately turning to prescription hormones. Evidence‑based natural strategies—cool‑environment techniques, symptom tracking, sleep hygiene, regular physical activity, avoidance of known triggers (caffeine, alcohol, spicy foods, smoking), mindfulness practices, and professional counseling—can meaningfully lessen hot flashes, night sweats, mood swings, and sleep disturbances while supporting overall well‑being. This article reviews the most reliable lifestyle and complementary options, explains how they fit together with medical treatments when needed, and offers practical steps women can take today to manage their symptoms safely and confidently.
Hormone‑Based and Non‑Hormonal Therapeutic Options
 Latest menopause treatments
The newest options for managing menopausal symptoms combine both hormone‑based and non‑hormonal therapies approved by the FDA. Hormone replacement therapy (HRT) remains the gold standard, with systemic combination (estrogen + progestogen) or estrogen‑only regimens delivered as pills, patches, gels, sprays, or vaginal rings, alongside low‑dose vaginal estrogen creams, tablets, or inserts for local dryness and pain. For women who cannot use estrogen, low‑dose antidepressants (SSRIs or SNRIs), gabapentin, and clonidine are effective for hot‑flash relief, while the recently approved neurokinin‑3 antagonist Fezolinetant (Veozah) offers a hormone‑free solution that targets the brain’s temperature‑regulation pathway. Intravaginal prasterone (Intrarosa) and oxybutynin (Oxytrol) provide additional options for vaginal atrophy and urinary urgency, respectively. Your provider can tailor a personalized regimen that balances symptom control with individual health risks and preferences.
Best menopause relief
The most effective relief for menopause symptoms is personalized hormone therapy, which can significantly reduce hot flashes, night sweats, and vaginal dryness while also protecting bone health. For women who cannot or choose not to use hormones, low‑dose antidepressants (SSRIs or SNRIs), gabapentin, or the newer non‑hormonal drug fezolinetant are proven alternatives that alleviate hot flashes. Vaginal estrogen products—creams, tablets, or rings—provide targeted relief for dryness and pain during intercourse with minimal systemic exposure. Over‑the‑counter supplements such as Asian ginseng, L‑theanine, and pollen extract may offer modest benefits for mood, sleep, or libido, but they lack robust evidence and should be discussed with a clinician first. Finally, lifestyle tweaks—identifying triggers, staying cool with fans and layered clothing, and staying well‑hydrated—can further lessen the intensity of menopausal symptoms.
The 3‑Day Menopause Reset Nutrition Plan
 What is the 3‑Day Menopause Reset? The 3‑Day Menopause Reset is a short‑term, structured nutrition program designed for perimenopausal and menopausal women. Over three days the program emphasizes three balanced meals per day—breakfast, lunch, and dinner—while eliminating between‑meal snacking to keep blood‑sugar levels steady. Each meal is built around high‑quality protein, vitamin‑rich vegetables, and low‑glycemic carbohydrates, which together help curb cravings, smooth energy swings, and promote the use of stored fat for fuel. Women who try the reset often report steadier mood, fewer afternoon slumps, and modest weight loss after the three‑day cycle. The plan is intended as a quick, organized “reset” that can be repeated or followed by longer‑term dietary habits for ongoing women’s‑health support.
Foods that help with menopause naturally Whole foods rich in phytoestrogens, omega‑3 fatty acids, and vitamin E can ease menopausal symptoms. Incorporate soy products (tofu, edamame, soy milk) and ground flaxseed, which provide isoflavones and lignans that may reduce hot flashes and night sweats. Cold‑water fish such as salmon, mackerel, or sardines supply anti‑inflammatory omega-3s that support mood and cardiovascular health. Leafy greens, berries, and other colorful vegetables deliver antioxidants, calcium, and vitamin D for bone support. Nuts, seeds, and whole grains add fiber, healthy fats, and vitamin E, further assisting hormone balance and skin health. Finally, limit caffeine, alcohol, and highly processed foods, as these can trigger vasomotor symptoms and disrupt sleep. By centering the reset around these nutrient‑dense choices, women can naturally mitigate many menopause‑related discomforts while laying the groundwork for long‑term wellness.
Evidence‑Based Natural Treatments
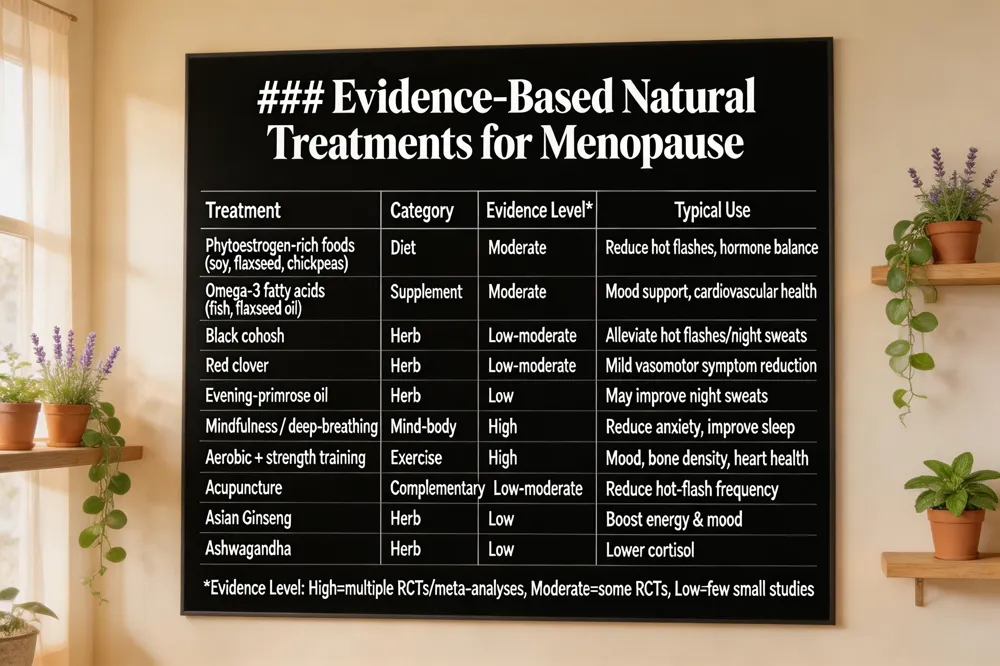 7 natural menopause treatments that really work A nutrient‑dense diet emphasizing whole foods, phytoestrogen sources (soy, flaxseed, chickpeas) and adequate calcium and vitamin D supports bone health and can lessen vasomotor symptoms. Regular aerobic activity combined with strength training and flexibility work (yoga, tai chi) improves mood, reduces hot‑flash frequency and maintains weight. Herbal options such as black cohosh, red clover and evening‑primrose oil have modest evidence for easing hot flashes and night sweats when taken under professional supervision. Mind‑body practices—mindfulness meditation, deep‑breathing, paced breathing—lower anxiety, improve sleep quality and reduce brain‑fog. Omega‑3 fatty acids and proper hydration help control inflammation and cardiovascular risk.
Natural remedies for menopause hot flashes Avoid known triggers (caffeine, alcohol, spicy foods) and dress in breathable, layered clothing to cool quickly. Gentle exercise, yoga, meditation or paced breathing reduces stress, a key aggravator of flashes. Acupuncture shows modest benefit in clinical trials. Incorporate phytoestrogen‑rich foods (soy, flaxseed) and consider herbs like black cohosh, red clover or evening‑primrose oil after consulting a clinician. Keep a symptom diary to identify personal patterns.
Natural remedies for menopause fatigue Support energy with low‑impact exercise (walking, yoga, tai chi) that improves circulation and sleep. Herbal choices such as black cohosh, evening‑primrose oil and ginseng may help, though doses are not standardized. A balanced diet rich in whole grains, lean protein and adequate hydration stabilizes blood‑sugar; limit caffeine and alcohol. Prioritize sleep hygiene (cool, dark bedroom, consistent bedtime) and stress‑reduction techniques.
Natural remedies for menopause anxiety Herbs like black cohosh, red clover, evening‑primrose oil, ginseng and angelica are used, but evidence is limited and drug interactions possible. Probiotic supplements may improve the gut‑brain axis. Regular aerobic, strength and mind‑body exercise (yoga) boost endorphins. Ashwagandha, an adaptogen, is sometimes recommended; discuss dosage with a provider. Cognitive‑behavioral therapy offers reliable, evidence‑based anxiety relief.
Natural remedies for menopause weight gain Herbal supplements (black cohosh, red clover, evening‑primrose oil, ginseng) aim to support hormonal balance and metabolism. Green‑tea catechins and cinnamon may modestly increase fat oxidation. Strength‑training preserves muscle mass, essential for resting metabolism. A whole‑food diet high in fiber and protein stabilizes blood sugar and curbs cravings. Always consult a menopause specialist before starting any supplement regimen.
Lifestyle Strategies for Symptom Management
 Menopause is a natural transition, but the accompanying vasomotor, mood, and sleep disturbances can feel overwhelming. A patient‑centered, evidence‑based lifestyle plan can ease many of these symptoms without immediately resorting to medication.
How to combat menopause symptoms naturally – Consistent sleep hygiene is a cornerstone: keep a dark, cool bedroom (≈18 °C/65 °F), go to bed at the same time each night, and limit caffeine, alcohol, and screen use before sleep. Dress in layers, choose breathable natural fabrics, and use fans or cool showers during a hot flash. A balanced diet rich in calcium (milk, yogurt, kale) and vitamin D (sun exposure or 400‑800 IU supplements) supports bone health, while phytoestrogen‑rich foods such as soy, flaxseed, and legumes may modestly reduce hot‑flash frequency. Regular aerobic activity (≥150 min/week) plus weight‑bearing or strength training improves mood, promotes weight management, and can lower the intensity of vasomotor symptoms. Mind‑body practices—yoga, tai chi, meditation, or cognitive‑behavioral therapy—lower stress and improve sleep quality.
How to stop menopause from happening – Menopause is an inevitable, irreversible phase of aging; it cannot be halted. However, maintaining a healthy weight, avoiding smoking, and managing stress may modestly delay onset. Early menopause risk factors (genetics, certain medical treatments) should be discussed with a qualified OB‑GYN, who can monitor hormone levels and offer supportive therapies.
How to lower cortisol in menopause – Prioritize sleep, practice daily mindfulness or deep‑breathing, and engage in regular aerobic and strength‑training exercise, all of which have been shown to reduce cortisol. A diet rich in magnesium (nuts, seeds, legumes), omega‑3 fatty acids (fatty fish, flaxseed oil), and protein supports hormonal balance. Social support, physical affection, and limiting caffeine/alcohol in the evening further help keep cortisol in check.
How to control menopause naturally – Combine the above strategies: keep a cool environment, track symptom patterns, avoid known triggers (spicy foods, caffeine, alcohol, smoking), and consider professional guidance before using any herbal supplements such as black cohosh or evening primrose oil, which have mixed evidence and may interact with medications. A personalized, step‑wise approach—starting with lifestyle foundations, adding targeted natural therapies, and consulting a healthcare provider when needed—offers the most reliable relief and promotes overall well‑being.
Diagnostic and Monitoring Tools

How to confirm menopause
Menopause is confirmed when a woman has experienced 12 consecutive months without a menstrual period with no other explanation such as pregnancy, medication, or illness. A clinician first evaluates the menstrual pattern and common vasomotor symptoms (hot flashes, night sweats) and genital changes (vaginal dryness). Laboratory testing may be used: elevated follicle‑stimulating hormone (FSH) and reduced estradiol levels are typical, while thyroid‑stimulating hormone (TSH) helps rule out thyroid disease. Home urine FSH kits can suggest a transition but are not definitive because levels fluctuate. The final diagnosis relies on the 12‑month criterion combined with clinical assessment and, when needed, blood tests.
What are the 34 symptoms of menopause
Menopause can produce a broad spectrum of symptoms: hot flashes, night sweats, sleep disturbances, fatigue, mood swings, irritability, anxiety, depression, memory lapses (brain fog), difficulty concentrating, irregular menstrual bleeding or spotting, decreased libido, vaginal dryness, painful intercourse, urinary urgency or incontinence, breast tenderness, joint pain, muscle aches, weight gain or redistribution, bloating, abdominal distension, hair thinning or loss, skin dryness, facial flushing, palpitations, dizziness, headaches or migraines, tingling or numbness in extremities, altered taste and smell, dry mouth, and long‑term bone loss leading to osteoporosis. These comprise the 34 typical menopause symptoms.
Bone and Cardiovascular Health During Menopause
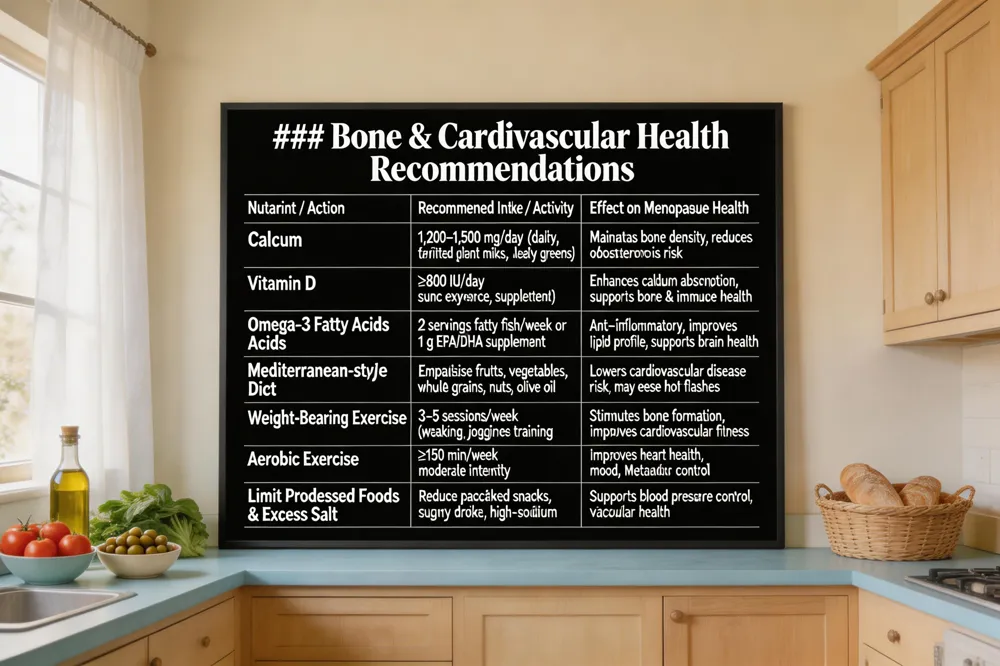 During menopause, declining estrogen accelerates bone loss and raises cardiovascular risk. Adequate calcium (1,200‑1,500 mg/day) and vitamin D (≥800 IU/day) support bone density, while a Mediterranean‑style diet, regular aerobic activity, and weight‑bearing exercise help maintain heart health and reduce hot‑flash frequency.
Menopause supplements Menopause supplements are widely marketed as natural remedies for hot flashes, night sweats, mood swings and other symptoms, but most have not been evaluated by the FDA and often lack solid clinical evidence of effectiveness or safety. Harvard experts caution that many of these products are supported more by celebrity endorsements than by rigorous research, and some may contain ingredients that interact with prescription medications. If you’re considering a supplement, look for third‑party testing and discuss it with a qualified clinician. A personalized approach—combining lifestyle modifications, evidence‑based hormone therapy when appropriate, and targeted nutrition—often yields the most reliable relief.
Natural remedies for menopause fatigue Menopause‑related fatigue can often be eased with a combination of gentle herbs and lifestyle tweaks. Herbal options such as black cohosh, evening primrose oil, and ginseng are commonly used to support energy and balance hormonal fluctuations, though doses aren’t standardized and you should check with a clinician before starting. Regular low‑impact exercise—like walking, yoga, or tai chi—helps improve circulation and sleep quality, which in turn reduces daytime tiredness. A balanced diet rich in whole grains, lean protein, plenty of water, and limited caffeine or alcohol can stabilize blood‑sugar levels and prevent energy crashes. Prioritizing good sleep hygiene (cool, dark bedroom, consistent bedtime routine) and managing stress through meditation or deep‑breathing further combats exhaustion.
Supporting Partners and Emotional Well‑Being
 Educate yourself about what menopause entails—its hormonal shifts, common symptoms (hot flashes, mood changes, sleep disturbances, reduced libido), and how they can affect your partner’s mood and energy levels. Keep open, non‑judgmental communication: ask how she’s feeling, listen without trying to “fix” everything, and let her know you’re there for her. Take care of your own health by staying active, eating a balanced diet, getting enough sleep, and managing stress, which will help you remain patient and supportive. Encourage professional help when needed, such as a gynecologist, therapist, or menopause specialist, and consider joint counseling to navigate any relational strain. Finally, nurture intimacy in ways that respect her comfort—focus on emotional connection, gentle touch, and flexible sexual expectations while she adjusts to the changes.
Conclusion
In summary, the seven evidence‑based natural approaches that consistently ease menopausal discomfort are: (1) creating a cool environment—layered breathable clothing, fans, and cool rooms; (2) tracking symptoms to identify personal triggers; (3) practicing good sleep hygiene with a dark, cool bedroom and a regular bedtime; (4) engaging in regular aerobic and strength‑training exercise; (5) avoiding known aggravators such as caffeine, alcohol, spicy foods, and smoking; (6) incorporating mindfulness‑based stress‑reduction techniques like yoga, meditation, or paced breathing; and (7) seeking professional counseling or therapy for mood, anxiety, or sexual concerns. While these strategies can be highly effective, their success is maximized when tailored to each woman’s unique health profile and goals. Our team in Queens is ready to partner with you, review your symptom diary, and design a personalized, clinician‑guided plan that may also include hormone therapy or other medical options when appropriate. Schedule a consultation today to begin your journey toward smoother, healthier menopause.





.png)