The Truth About Birth Control Pills: What Medical Experts Want You to Know

Understanding Fibroid Treatments
Uterine fibroids affect 70–80 % of pre‑menopausal women in the United States, often causing heavy bleeding, pelvic pain, and infertility concerns. Diagnosis begins with a pelvic exam followed by imaging—transabdominal or transvaginal ultrasound is the first line, while MRI or hysterosonography clarifies size, number, and location for treatment planning. Shared decision‑making should integrate symptom severity, desire for future fertility, and personal health goals. Discuss the full spectrum of options: hormonal therapies (e.g., GnRH agonists, LNG‑IUD) for short‑term control; uterus‑preserving procedures such as myomectomy, uterine artery embolization, or MRI‑guided focused ultrasound; and definitive hysterectomy when childbearing is complete. Consider recovery time, potential risks, cost, and the impact on quality of life to choose the approach that aligns with each woman’s values. Open dialogue with a gynecologist ensures the plan reflects both medical evidence and personal preferences.
Hormonal Therapies: Options, Efficacy, and Side Effects
 Uterine fibroids respond to several hormone‑based medicines that aim to shrink the tumors or control bleeding. GnRH agonists and antagonists such as leuprolide (Lupron) or elagolix create a temporary menopause‑like state, lowering estrogen and progesterone. Agonists are usually given by injection for 3‑6 months and can reduce fibroid volume by 30‑50 %, while antagonists can be taken orally for up to two years with fewer hot‑flash symptoms. Oral tablet options include GnRH antagonists (relugolix/estradiol/norethindrone) and, experimental agents like linzagolix (Yselty) that have demonstrated measurable shrinkage. Conventional birth‑control pills lessen bleeding but do not shrink fibroids, and ulipristal carries rare liver‑injury warnings. Levonorgestrel‑releasing IUDs (Mirena) thin the endometrium, dramatically decreasing menstrual loss, yet they do not reduce fibroid size and may be unsuitable when the uterine cavity is distorted. Hormone‑replacement considerations: after hysterectomy or during menopause, low‑dose progestin‑only regimens or GnRH‑based add‑back therapy can protect bone density while keeping estrogen low enough to avoid stimulating fibroid growth. Nutritional support: a Mediterranean‑style diet rich in leafy greens, berries, green tea, probiotic yogurt, eggs, omega‑3 fish, and nuts supplies antioxidants and anti‑inflammatory compounds that may aid hormone balance and modestly shrink fibroids. Tablets to shrink fibroids – Yes, oral GnRH antagonists (e.g., elagolix) and experimental linzagolix can reduce size; traditional pills cannot. Best hormonal treatment – Short‑term GnRH agonists (leuprolide) provide the greatest shrinkage before surgery. Side‑effects – Hot flashes, night sweats, bone loss, mood changes, spotting, weight gain, and rare clot risks; monitoring is essential. Can you take HRT with fibroids? – Yes, but low‑dose estrogen‑limiting regimens (progestin‑only or GnRH‑based) are preferred to avoid stimulating growth. 7 foods for shrinking fibroids – Spinach, kale, berries, green tea, yogurt, eggs, salmon, and nuts, eaten regularly, support hormone metabolism and may lessen fibroid size.
Surgical Options: Myomectomy vs. Hysterectomy
 Uterine fibroids affect 70‑80 % of pre‑menopausal women in the United States, and the choice of surgery hinges on fertility goals, symptom severity, and long‑term health risks.
Myomectomy techniques and fertility preservation – Myomectomy removes only the fibroids while sparing the uterus, making it the gold‑standard for women who wish to conceive. It can be performed hysteroscopically for submucosal lesions, laparoscopically or robot‑assisted for intramural or subserosal tumors, or via a traditional laparotomy for very large or numerous fibroids. Minimally invasive approaches reduce blood loss, limit scarring, and typically allow a return to normal activities within two to six weeks.
Hysterectomy as definitive cure – Hysterectomy eliminates the uterus and all fibroids, providing permanent symptom relief and eliminating recurrence. It is reserved for women who have completed childbearing, have severe refractory bleeding, or when malignancy is suspected.
Cost‑effectiveness and coronary artery disease (CAD) risk – A Mayo Clinic simulation of 10,000 U.S. women aged 40 showed myomectomy to be more cost‑effective than hysterectomy while delivering comparable quality‑of‑life benefits. Hysterectomy was associated with up to a 33 % higher odds of CAD compared with myomectomy, underscoring the importance of weighing cardiovascular risk in treatment planning.
Recovery timelines by surgical approach – Minimally invasive hysterectomy (laparoscopic, robotic, or vaginal) often requires an overnight stay and a two‑to‑four‑week recovery, whereas an open abdominal hysterectomy can extend convalescence to six weeks. Myomectomy recovery varies: hysteroscopic and laparoscopic cases heal in 2‑4 weeks, while open myomectomy may need 4‑6 weeks.
Key patient‑focused questions –
- Gold‑standard treatment? Hysterectomy offers a definitive cure; myomectomy is preferred for fertility preservation.
- Pros and cons of hysterectomy? Immediate symptom resolution vs. surgical risks and loss of fertility.
- When to consider hysterectomy? Severe, unrelenting symptoms or completion of childbearing.
- Recovery time? Varies by method; minimally invasive techniques recover fastest.
- Best treatment for large fibroids? Myomectomy (laparoscopic/robotic) if fertility is desired; hysterectomy if not.
- Shrink vs. remove? Surgical removal is indicated for infertility, severe pain, or refractory bleeding; medical shrinkage is useful for short‑term symptom control when fertility must be preserved.
Choosing the optimal pathway involves shared decision‑making with a trusted OB/GYN, integrating personal goals, health status, and the latest evidence.
Minimally Invasive and Non‑Surgical Innovations
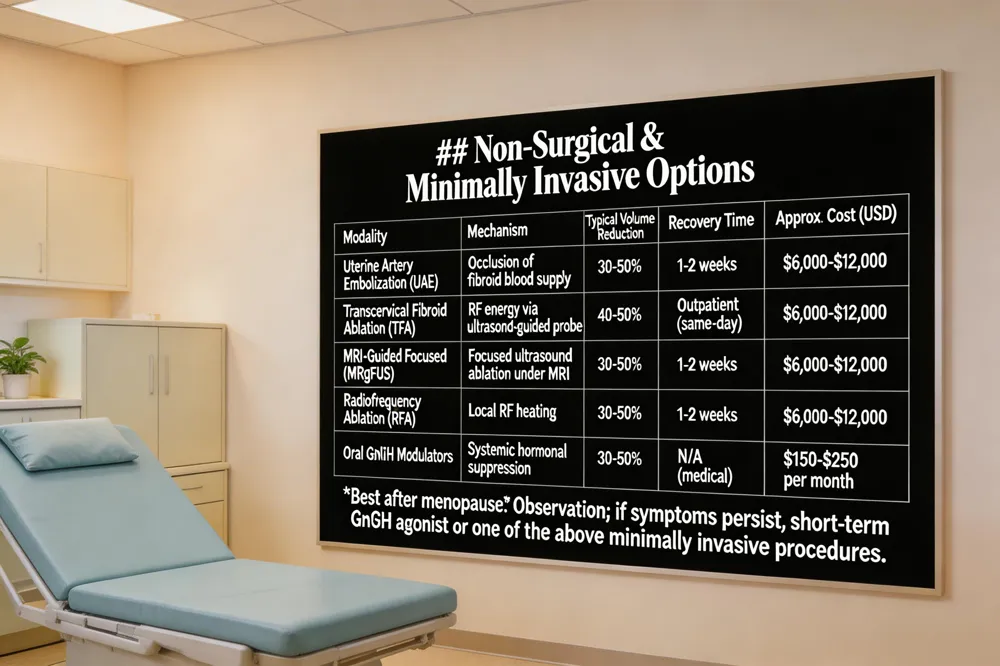 Uterine fibroids are traditionally treated with surgery, but a growing portfolio of uterus‑preserving options now lets many women avoid incisions.
Uterine artery embolization (UAE) blocks fibroid blood flow with tiny particles delivered through a catheter, shrinking lesions by 30‑50 % and relieving heavy bleeding. Recovery is usually 1‑2 weeks, and most insurers cover the procedure when medically indicated.
Transcervical fibroid ablation (TFA) uses a thin, ultrasound‑guided probe inserted through the vagina to deliver radio‑frequency energy that contracts fibroid tissue by 40‑50 %. It is an outpatient, incision‑free option that rapidly eases bleeding and pelvic pain.
MRI‑guided focused ultrasound (MRgFUS) focuses high‑energy sound waves on fibroids under MRI guidance, thermally ablating tissue without any incision. Although effective, insurance coverage can be variable, making it less accessible for some patients.
Radiofrequency ablation (RFA) techniques—whether transcervical or laparoscopic—offer similar volume reduction with short recovery times and uterus preservation.
New treatment for fibroids without surgery: TFA and other RFA methods provide a cutting‑edge, non‑surgical alternative that eliminates stitches and hospital stays, delivering symptom relief within weeks.
Cost: UAE, RFA and MRgFUS typically range from $6,000‑$12,000 per treatment; oral hormone modulators (e.g., Oriahnn, Myfembree) average $150‑$250 per month.
Best after menopause: Most fibroids shrink naturally; observation is often sufficient. Persistent symptoms may be managed with short‑term GnRH agonists or minimally invasive procedures like TFA, UAE, or endometrial ablation.
Overall treatment pathway: Begin with watchful waiting, then consider hormonal therapy, followed by minimally invasive options (UAE, MRgFUS, RFA/TFA) before surgical myomectomy or hysterectomy, based on symptom severity, fibroid characteristics, and fertility goals.
FIGO Classification Guided Management
 Uterine fibroids are classified by FIGO type, which directs a location‑specific treatment strategy while balancing fertility goals and symptom control.
FIGO 1 (submucosal, intracavitary) – These lesions often cause heavy bleeding and infertility. Initial management favors medical therapy—GnRH antagonists, oral progestins, or a levonorgestrel‑releasing IUD to reduce bleeding and shrink the fibroid. If uterine preservation is desired, hysteroscopic resection is the preferred surgical option, allowing precise removal with minimal uterine trauma. A combined pre‑operative GnRH antagonist followed by hysteroscopic or laparoscopic surgery enhances outcomes when the fibroid is large.
FIGO 2 (submucosal, partially intracavitary) – GnRH antagonists (e.g., relugolix) rapidly lower volume and improve anemia while preserving fertility. Short‑term GnRH agonists can be used pre‑operatively. Levonorgestrel‑IUDs, combined oral contraceptives, or tranexamic acid control bleeding. When medical therapy is insufficient, hysteroscopic resection remains the minimally invasive surgical choice.
FIGO 3 (intramural, no cavity involvement) – Initial therapy includes GnRH antagonists, LNG‑IUDs, or tranexamic acid for bleeding control. Persistent symptoms or fertility wishes may be addressed with minimally invasive myomectomy (laparoscopic, robotic, or hysteroscopic). Larger or multiple lesions can be managed with uterine artery embolization or MRI‑guided focused ultrasound. Hysterectomy is reserved for definitive cure after childbearing.
FIGO 6 (subserosal pedunculated) – Surgical removal, typically laparoscopic myomectomy or hysterectomy when fertility is not a concern, is the definitive option. Pre‑operative GnRH antagonists or LNG‑IUDs can reduce size and bleeding. Minimally invasive alternatives such as uterine artery embolization or MRI‑guided focused ultrasound are viable when surgery is contraindicated. Multidisciplinary, patient‑led counseling ensures the chosen pathway aligns with individual reproductive plans and health status.
Lifestyle, Monitoring, and Patient Empowerment
 Effective self‑care starts with regular symptom tracking. Keep a diary of menstrual flow, pelvic pressure, urinary frequency and any new abdominal swelling; these clues often signal fibroid growth. Nutrition can support overall health—high‑fiber foods, leafy greens, and vitamin D‑rich sources may help reduce inflammation, while limiting excess red meat and sugary drinks may lessen estrogen‑driven fibroid expansion.
Home palpation is a simple, low‑risk way to sense changes. Lie on your back, place a pillow under your knees, and using the pads of your fingers, press gently just below the belly button. A firm, irregular lump that feels different from the surrounding tissue could be a fibroid; note its size, tenderness, and any shift over weeks.
Visual expectations after treatment are often striking. Before‑and‑after photos typically show a disappearance of the “fibroid belly,” with a flatter waistline and smoother abdominal contour after myomectomy, embolization, or radio‑frequency ablation.
Which size of fibroid is dangerous? Large fibroids ≥ 10 cm can compress organs, cause heavy bleeding and pain, and affect fertility; medium‑size (5‑10 cm) may also become problematic depending on location and symptom severity. Small fibroids (< 2 cm) are usually harmless.
How to check for fibroids at home? Monitor heavy periods, pelvic pressure, and urinary changes; perform gentle self‑palpation as described above and record any palpable masses or pain. Share findings with your OB/GYN for imaging confirmation.
Before and after pictures of fibroid removal illustrate a reduced lower‑abdominal bulge and a return to normal uterine size, highlighting both cosmetic and symptom relief.
What is the fastest way to shrink fibroids? Short‑term GnRH‑agonist therapy (e.g., leuprolide) can cut fibroid volume by 30‑50 % in 2‑3 months; GnRH antagonists or selective progesterone‑receptor modulators (relugolix, ulipristal) also shrink fibroids quickly, while minimally invasive procedures like uterine artery embolization or radio‑frequency ablation deliver rapid size reduction without long‑term medication.
Personalized, Women‑Led Care in Queens
Women in Queens deserve a treatment plan that blends hormonal medicines, minimally invasive procedures, and definitive surgery, all chosen with their unique goals in mind. Short‑term GnRH agonists or antagonists can shrink fibroids and reduce bleeding before a myomectomy, while a levonorgestrel‑releasing IUD eases heavy flow for smaller lesions. For those who wish to preserve fertility, myomectomy—performed hysteroscopically, laparoscopically, or robotically—offers symptom relief with a low recurrence risk, whereas uterine artery embolization or transcervical radiofrequency ablation provide uterus‑sparing alternatives for larger or multiple fibroids. Women who have completed childbearing may opt for a hysterectomy, which eliminates recurrence but carries a higher odds of later coronary artery disease. Ongoing imaging, symptom tracking, and open dialogue between patient and multidisciplinary team ensure that each decision reflects current health status, symptom severity, and future family plans.





.png)