The Truth About Birth Control Pills: What Medical Experts Want You to Know
A Guided Journey Through Prenatal Testing: Empowering Your Choices
Prenatal tests are an important part of modern pregnancy care. They provide valuable information about the baby's health and development before birth. Many tests also check the mother's health. The goal is to give expectant parents and their healthcare team the knowledge needed for informed decisions and personalized care.
Types of Prenatal Tests: Screening vs. Diagnostic
It is crucial to understand the difference between screening and diagnostic tests. They serve very different purposes. Screening tests assess the chance or risk that a baby might have a certain genetic condition or birth defect. They are not perfect and cannot provide a definitive yes-or-no answer. A positive screening result indicates a higher-than-average risk. A negative result suggests a lower risk. These tests are typically non-invasive, involving blood draws from the mother and ultrasound exams. Diagnostic tests, on the other hand, can confirm whether a baby has a specific genetic condition. They provide a definitive diagnosis. These tests involve analyzing fetal cells obtained through procedures like chorionic villus sampling (CVS) or amniocentesis. Because they are invasive, they carry a small risk of complications, including miscarriage.
Understanding the Common Conditions Screened
Prenatal tests focus on detecting specific types of health conditions. The most common targets are chromosomal abnormalities and neural tube defects. Chromosomal abnormalities involve missing or extra chromosomes. Down syndrome (trisomy 21) is the most common, occurring in about 1 in 800 live births. Other conditions include Edwards syndrome (trisomy 18) and Patau syndrome (trisomy 13). The risk of these abnormalities increases with maternal age. Neural tube defects are birth defects of the brain and spine, such as spina bifida. Screening also looks for certain inherited genetic disorders, like cystic fibrosis or sickle cell disease, often through separate carrier screening of the parents.
Timeline: When Are Tests Typically Offered?
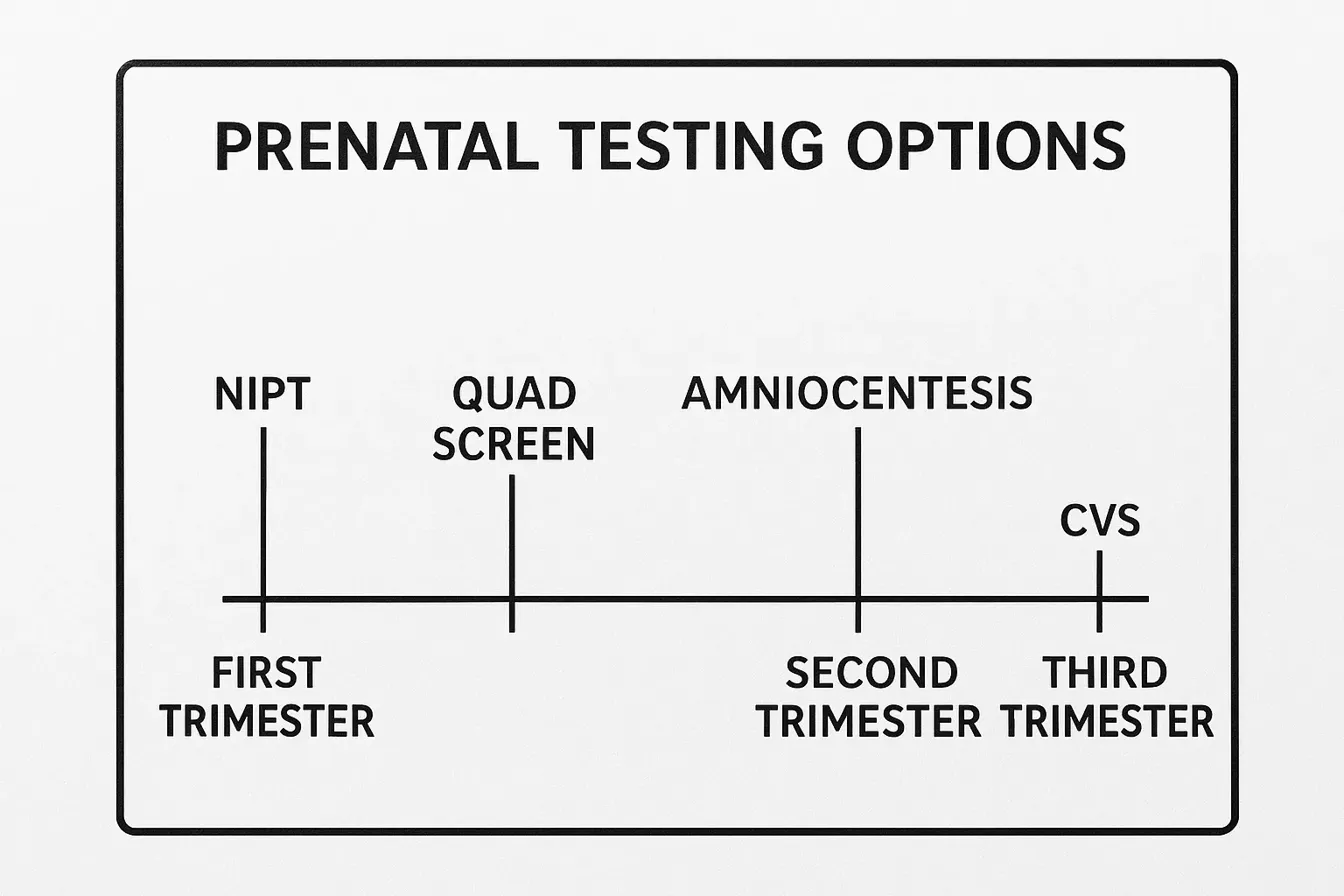
Prenatal testing follows a schedule aligned with pregnancy milestones. Different tests are offered at specific times for optimal accuracy and decision-making. The first trimester (weeks 1-13) includes initial blood work and early screening options. The second trimester (weeks 14-27) offers more screening and the timing for key diagnostic procedures. The third trimester focuses on maternal health and fetal well-being. This structured timeline allows for a stepwise approach, where screening results can guide the potential need for more definitive diagnostic testing.
Diving Deeper into First and Second Trimester Screening
First trimester screening usually occurs between weeks 10 and 13. It often combines a maternal blood test with a special ultrasound called a nuchal translucency (NT) scan. The blood test measures specific pregnancy hormones. The NT ultrasound measures the clear space at the back of the baby's neck. Together, they assess the risk for Down syndrome and trisomy 18. Second trimester screening is frequently done between weeks 15 and 22. A common test is the quad screen, a blood test that measures four different substances. It evaluates risk for Down syndrome, trisomy 18, and neural tube defects. A routine anatomy ultrasound, usually between 18 and 22 weeks, is also recommended for every pregnancy to check the baby's physical development.
The Role of Ultrasounds and Non-Invasive Prenatal Testing (NIPT/cfDNA)
Ultrasound is a versatile, non-invasive imaging tool used throughout pregnancy. In the first trimester, it confirms the due date and can be part of NT screening. The mid-pregnancy anatomy scan examines fetal structures in detail. Ultrasounds can detect many physical abnormalities but cannot diagnose genetic conditions on their own. Non-Invasive Prenatal Testing (NIPT), also called cell-free DNA (cfDNA) screening, is a significant advance. This is a blood test that analyzes tiny fragments of the baby's DNA circulating in the mother's bloodstream. It can be done as early as 10 weeks into pregnancy. NIPT is highly accurate for screening common chromosomal conditions like Down syndrome. It can also reveal the baby's sex. It is important to remember that NIPT is still a screening test, not a diagnostic one.
Navigating Results, Risks, and the Importance of Counseling
Understanding test results is a key part of the process. A screening test result is usually given as a risk level (e.g., high-risk or low-risk). It is not a diagnosis. All screening tests have rates of false-positive and false-negative results. A false-positive means the test suggests a high risk when the baby is actually unaffected. This can cause unnecessary anxiety. Diagnostic tests like CVS and amniocentesis have high accuracy (over 99%) but carry a small procedure-related risk of miscarriage—about 1 in 450 for CVS and 1 in 900 for amniocentesis when performed by an expert. Weighing these potential risks against the benefit of a definitive answer is a personal decision. Genetic counseling is a vital resource. A genetic counselor is a healthcare professional who helps interpret test results, explains risks in clear terms, and discusses options without pressure. They provide support tailored to your family's history, values, and goals. Professional guidelines recommend that all patients receive counseling about their prenatal testing options.
| Test Type | Common Examples | Primary Purpose | Typical Timing | Key Consideration |
|---|---|---|---|---|
| Screening | First Trimester Screen, Quad Screen, NIPT/cfDNA | Assess risk of genetic conditions/birth defects | 10-13 wks, 15-22 wks, from 10 wks | Results indicate probability, not a diagnosis |
| Diagnostic | Chorionic Villus Sampling (CVS), Amniocentesis | Provide a definitive diagnosis of genetic conditions | 10-14 wks, 15+ wks | Carries a small risk of pregnancy loss |
| Imaging | Nuchal Translucency Ultrasound, Anatomy Ultrasound | Check physical development and anatomy | 11-14 wks, 18-22 wks | Cannot diagnose genetic conditions alone |
| Maternal Health | Glucose Test, Group B Strep Culture | Screen for conditions in the mother | 24-28 wks, 35-37 wks | Important for managing pregnancy health |
A Guided Journey Through Prenatal Testing: Empowering Your Choices

Introduction to Prenatal Screening and Testing
Prenatal testing provides valuable information about your baby's health during pregnancy. These optional tests help identify the risk or presence of certain genetic conditions, chromosomal abnormalities, and structural birth defects. The primary goal is to empower you and your healthcare team to make informed decisions, plan for potential medical needs, and optimize care both during pregnancy and after your baby is born. Even if a condition cannot be treated before birth, having this information allows time for emotional preparation and logistical planning.
Types of Prenatal Tests: Screening vs. Diagnostic
A critical distinction in prenatal testing is between screening tests and diagnostic tests.
- Screening tests estimate the chance or probability that your baby might have a specific condition. They are generally non-invasive, involving a blood draw from the mother or an ultrasound exam. Screening tests, such as the first-trimester screening or the quad screen, cannot provide a definitive 'yes' or 'no' diagnosis. Instead, their results are reported as a risk level—such as 'increased risk' or 'reduced risk.'
- Diagnostic tests can provide a definitive answer about whether your baby has a specific genetic condition. These procedures, such as chorionic villus sampling (CVS) and amniocentesis, are more invasive and involve taking a small sample of placental tissue or amniotic fluid. While highly accurate, they carry a small risk of pregnancy loss, which is an important factor to discuss with your provider.
'What is prenatal screening, and what are the four main types of prenatal tests?'
Prenatal screening involves a series of optional tests during pregnancy that assess the risk of certain genetic conditions and birth defects in the fetus. The four main types of prenatal tests are:
- First-trimester screening: This combines a maternal blood test measuring pregnancy-associated plasma protein A (PAPP-A) and human chorionic gonadotropin (hCG) with a nuchal translucency ultrasound. The ultrasound measures the clear space at the back of the baby’s neck. This screening, done between weeks 10 and 13, assesses risk for Down syndrome and trisomy 18.
- Second-trimester screening (Quad screen/Multiple marker): This is a maternal blood test performed between 15 and 22 weeks. It measures four substances (alpha-fetoprotein or AFP, hCG, estriol, and inhibin A) to evaluate risk for Down syndrome, trisomy 18 (Edwards syndrome), and open neural tube defects like spina bifida.
- Cell-free DNA testing (NIPT/NIPS): This is a highly accurate screening blood test that analyzes fetal DNA fragments circulating in the mother’s blood. It can be done as early as 10 weeks and screens for specific chromosomal conditions like Down syndrome, trisomy 18, and trisomy 13 (Patau syndrome). It can also determine the baby's sex and screen for certain sex chromosome differences.
- Diagnostic procedures: These include amniocentesis and chorionic villus sampling (CVS). They provide a confirmed diagnosis by analyzing fetal cells from amniotic fluid or placental tissue, respectively. They are typically offered after a high-risk screening result or due to other risk factors.
Understanding the Common Conditions Screened
Prenatal tests primarily focus on detecting chromosomal abnormalities, neural tube defects, and other structural issues.
- Chromosomal Abnormalities: These occur when a baby has missing or extra chromosomes. The most common is trisomy 21 (Down syndrome), occurring in about 1 in 700 births. Other conditions include trisomy 18 (Edwards syndrome) and trisomy 13 (Patau syndrome). The risk for these increases with maternal age.
- Neural Tube Defects (NTDs): These are birth defects of the brain and spine, such as spina bifida and anencephaly. They are often screened for by measuring the level of alpha-fetoprotein (AFP) in the mother’s blood during the second trimester.
- Inherited Genetic Disorders: Carrier screening is a separate type of test for parents, ideally done before or early in pregnancy. It checks if you or your partner carry a gene for conditions like cystic fibrosis, spinal muscular atrophy, sickle cell disease, or Tay-Sachs disease, which could be passed to your baby.
Timeline: When Are Tests Typically Offered?
Testing is offered at specific times throughout pregnancy to ensure accuracy and relevance. A general timeline is provided below.
| Pregnancy Trimester | Week Range | Common Tests Offered | Primary Purpose of Testing |
|---|---|---|---|
| First Trimester | 10-13 weeks | First-trimester screening, CVS, cfDNA/NIPT | Early risk assessment for chromosomal conditions. CVS provides early diagnosis. |
| Second Trimester | 15-22 weeks | Quad screen, Anatomy ultrasound, Amniocentesis | Broader risk assessment for chromosomal & neural tube defects. Anatomy scan checks for physical abnormalities. |
| Mid-to-Late Pregnancy | 24-28 weeks & 35-37 weeks | Glucose challenge test, Group B Strep culture | Screen for gestational diabetes and check for bacteria that could affect the newborn. |
| Throughout | As needed | Routine ultrasounds, Blood pressure/urine checks | Monitor fetal growth, position, and maternal health for conditions like preeclampsia. |
Diving Deeper into First and Second Trimester Screening
First-Trimester Screening: This early assessment is valuable for providing information sooner. An abnormal nuchal translucency measurement (greater than 3 mm) may indicate a higher risk not only for chromosomal issues but also for some fetal heart defects, often prompting a recommendation for a specialized fetal echocardiogram.
Second-Trimester Quad Screen: This test is often recommended if first-trimester screening was not performed. An abnormal AFP level can signal a potential neural tube defect or an abdominal wall defect, leading to a recommendation for a detailed, high-level ultrasound for further evaluation.
Combined or Sequential Screening: Some screening strategies integrate results from both the first and second trimesters to increase the overall detection rate for conditions like Down syndrome. Your provider can explain if this approach is suitable for you.
The Role of Ultrasounds and Non-Invasive Prenatal Testing (NIPT/cfDNA)
Ultrasounds are a cornerstone of prenatal care, using sound waves to create images of your baby. They are used to confirm dates, check growth, and, most importantly, examine fetal anatomy during the mid-pregnancy scan (around 18-22 weeks). This detailed anatomy survey looks at the brain, spine, heart, kidneys, limbs, and other structures to check for physical birth defects.
Cell-Free DNA Testing (NIPT/NIPS) represents a significant advance in screening. By analyzing placental DNA in the mother's blood, it offers very high accuracy for detecting common trisomies. Major medical organizations now recommend it be offered to all pregnant patients. It is crucial to understand that NIPT is still a screening test, not a diagnostic one. A 'high-risk' result requires follow-up with a diagnostic test like amniocentesis for confirmation.
Navigating Results, Risks, and the Importance of Counseling
Understanding Results: Screening test results explained are given as a risk assessment. A 'screen positive' or 'high-risk' result means the chance of the condition is higher than a certain cutoff; it is not a diagnosis. Conversely, a 'screen negative' or 'low-risk' result substantially reduces the likelihood but does not guarantee the baby is unaffected.
Considering Risks: The risks of testing vary. Screening tests like blood draws and ultrasounds pose no physical risk to the pregnancy. Diagnostic tests like amniocentesis and CVS are safe when performed by experienced specialists, but they do carry a small procedure-related risk of miscarriage (e.g., less than 1 in 900 for amniocentesis). Emotional risks, such as anxiety while waiting for results or after receiving a high-risk screening result, are also important to consider.
The Essential Role of Genetic Counseling: Consulting with a genetic counselor or your obstetrician is a key step. They can help you:
- Understand your personal risk factors based on age, family, and medical history.
- Interpret complex screening results and explain the difference between screening and diagnosis.
- Discuss the risks and benefits and limitations of each test to align with your personal values and goals for your pregnancy.
- Guide you through next steps if a test indicates an increased risk, including the option for diagnostic testing.
The decision to pursue any prenatal testing is deeply personal. There is no right or wrong choice, only the choice that is right for you and your family. Open conversation with your healthcare provider ensures you have the support and information needed to navigate this journey with confidence.
A Guided Journey Through Prenatal Testing: Empowering Your Choices

Introduction to Prenatal Screening and Testing
Prenatal testing provides valuable information about a baby's health during pregnancy. These tests help expectant parents understand potential genetic conditions or birth defects. This knowledge enables informed decisions about pregnancy management and future care plans. The goal is to address parental hopes and concerns, offering clarity and options. Importantly, prenatal tests are optional. Making an informed choice that aligns with personal values and healthcare goals is a crucial step for every family.
Types of Prenatal Tests: Screening vs. Diagnostic
A fundamental distinction exists between screening and diagnostic tests. Screening tests assess the risk or likelihood of a fetus having a disorder. They are non-invasive and typically involve blood tests and ultrasounds. A positive screening test result indicates a higher chance compared to the general population, but it is not a definitive diagnosis. Diagnostic tests, such as chorionic villus sampling (CVS) and amniocentesis, provide a definitive answer. They confirm whether a specific genetic condition is present. However, diagnostic procedures are invasive and carry a small risk of complications, including miscarriage.
Understanding the Common Conditions Screened
Prenatal tests focus on several types of genetic and structural conditions. Chromosomal abnormalities, known as aneuploidies, involve missing or extra chromosomes. The most common is Down syndrome (trisomy 21). Other conditions include Edwards syndrome (trisomy 18) and Patau syndrome (trisomy 13). Tests also screen for neural tube defects, such as spina bifida and anencephaly. Additionally, carrier screening can identify if parents carry genes for inherited disorders like cystic fibrosis, sickle cell disease, and spinal muscular atrophy.
| Condition Category | Specific Examples | Primary Test Types | Key Notes |
|---|---|---|---|
| Chromosomal Aneuploidies | Down syndrome (Trisomy 21) | Screening (NIPT, cell-free DNA screening, serum screening, Diagnostic (CVS, amnio) | Most common chromosomal disorder. |
| Chromosomal Aneuploidies | Edwards syndrome (Trisomy 18) | Screening (NIPT, quad screen), Diagnostic (CVS, amnio) | Often associated with severe abnormalities. |
| Neural Tube Defects | Spina bifida, Anencephaly | Second-trimester Maternal Serum Alpha-fetoprotein (MSAFP) screening, Anatomy ultrasound | Screened via alpha-fetoprotein (AFP) levels. |
| Inherited Genetic Disorders | Cystic fibrosis, Sickle cell | Carrier screening (parental blood test) | Tests parents before or during pregnancy. |
Timeline: When Are Tests Typically Offered?
Testing is tied to specific gestational windows to ensure accuracy and allow for timely decisions. Carrier screening is ideally done before conception or early in pregnancy. First-trimester screenings occur between 10 and 13 weeks. Second-trimester screenings, like the quad screen, are offered between 15 and 22 weeks. Diagnostic tests also have specific timeframes: CVS is performed between 10 and 14 weeks, while amniocentesis is done after 15 weeks. Later in pregnancy, screenings for gestational diabetes (24-28 weeks) and Group B Strep (35-37 weeks) are standard.
Diving Deeper into First and Second Trimester Screening
First-trimester screening combines a maternal blood test measuring specific proteins with a nuchal translucency (NT) ultrasound. The NT ultrasound measures the clear space at the back of the baby's neck. An increased measurement can indicate a higher risk for chromosomal conditions. Second-trimester screening often involves the "quad screen." This blood test measures four substances to assess risk for Down syndrome, trisomy 18, and neural tube defects. A routine anatomy ultrasound in the second trimester is also recommended for every pregnancy to check for physical structural abnormalities.
The Role of Ultrasounds and Non-Invasive Prenatal Testing (NIPT/cfDNA)
Ultrasound is a versatile, non-invasive imaging tool used throughout pregnancy. In the first trimester, it establishes accurate due dates. The mid-pregnancy anatomy scan (18-22 weeks) provides a detailed check of fetal development. Non-Invasive Prenatal Testing (NIPT), also called cell-free DNA (cfDNA) screening, is a significant advance. It is a blood test that analyzes fetal DNA from the placenta present in the mother's bloodstream. Available from 10 weeks onward, it screens with high sensitivity for conditions like Down syndrome and can also reveal fetal sex. It is a screening test, not diagnostic.
Navigating Results, Risks, and the Importance of Counseling
Understanding test results is vital. Screening tests report risk levels, not yes/no answers. A positive screening result means an increased risk, necessitating further discussion and possibly diagnostic testing for confirmation. All tests have limitations, including the possibility of false-positive or false-negative results. The emotional impact of testing, from anxiety while awaiting results to processing difficult news, is an important consideration. Consulting with a healthcare professional or a certified genetic counselor is essential. They provide personalized guidance, explain risks and benefits, and help interpret results to support your family's unique journey.
| Prenatal Test Overview | Typical Timing | Test Purpose | Key Considerations |
|---|---|---|---|
| Carrier Screening | Pre-pregnancy or early 1st trimester | Identifies parental gene carriers | Informs risk for inherited disorders. |
| First-Trimester Screen | 10-13 weeks | Combines NT ultrasound & blood test | Early risk assessment for aneuploidy. |
| NIPT / cfDNA Screening | From 10 weeks | Analyzes placental DNA in blood | High accuracy screen; not diagnostic. |
| Quad Screen | 15-22 weeks | Blood test measuring four markers | Screens for aneuploidy & neural tube defects. |
| Anatomy Ultrasound | 18-22 weeks | Detailed fetal structural exam | Recommended for every pregnancy. |
| Chorionic Villus Sampling | 10-14 weeks | Samples placental tissue | Diagnostic; carries miscarriage risk. |
| Amniocentesis | After 15 weeks | Samples amniotic fluid | Diagnostic; lower risk than CVS. |
A Guided Journey Through Prenatal Testing: Empowering Your Choices

Introduction to Prenatal Screening and Testing
Prenatal tests are a standard part of pregnancy care, designed to provide valuable information about your health and the health of your developing baby. These tests help identify potential issues early, allowing for informed decisions, medical planning, and often, reassurance. They are generally divided into two broad categories: screening tests and diagnostic tests. Screening assessments estimate risk, while diagnostic procedures provide definitive answers.
All pregnant individuals are offered these tests, but the choice to accept them is personal. There is no single right path; the best decision is one that aligns with your values, concerns, and medical circumstances, made with the support of your healthcare team.
Types of Prenatal Tests: Screening vs. Diagnostic
Understanding the fundamental difference between screening and diagnostic tests is crucial for navigating your options.
- Screening Tests: These are typically non-invasive tests that assess the statistical probability or chance that your baby might have a specific condition. They include blood tests and ultrasounds. A screening result does not provide a diagnosis. Instead, it classifies a pregnancy as having a lower or higher risk compared to the general population. It's important to know that screening tests are not perfect and can have false-positive results (indicating a risk when none exists) or false-negative results (missing an actual risk).
- Diagnostic Tests: These are procedures that can definitively diagnose whether a baby has a genetic condition. The most common are chorionic villus sampling (CVS) and amniocentesis. Because they involve sampling fetal cells, they carry a small procedural risk of pregnancy loss. Diagnostic testing is usually recommended after a high-risk screening result or due to specific risk factors like maternal age, family history, or concerning ultrasound findings.
Understanding the Common Conditions Screened
Prenatal testing primarily focuses on detecting certain chromosomal conditions and structural birth defects.
Chromosomal Conditions: These are caused by missing or extra chromosomes. The most common is Down syndrome (Trisomy 21). Others include Edwards syndrome (Trisomy 18) and Patau syndrome (Trisomy 13). The risk for many chromosomal conditions increases with maternal age.
Structural Birth Defects: These are physical abnormalities in development. A key focus is on neural tube defects, like spina bifida (an opening in the spine) and anencephaly. These are screened for by measuring a protein called alpha-fetoprotein (AFP) in the mother's blood during the second trimester.
Inherited Genetic Disorders: Carrier screening is a separate type of test performed on prospective parents to see if they carry a gene for conditions like cystic fibrosis, spinal muscular atrophy, or sickle cell disease. This helps assess the baby's risk of inheriting the disorder.
Timeline: When Are Tests Typically Offered?
Prenatal testing follows a structured schedule tied to gestational age to ensure accuracy and timely information.
| Trimester | Gestational Age Window | Common Tests & Screenings Offered | Primary Purpose |
|---|---|---|---|
| First | 6-13 weeks | Initial blood work, Carrier screening, First-trimester screening (blood test + nuchal translucency ultrasound | Confirm pregnancy, assess maternal health, early risk assessment for chromosomal conditions |
| Second | 15-22 weeks | Quad screen blood test, Detailed anatomy ultrasound, Diagnostic tests (amniocentesis from 15 weeks) | Screen for chromosomal conditions & neural tube defects, check fetal anatomy, provide definitive diagnosis if needed |
| Third | 24-37 weeks | Glucose challenge test, Group B Strep culture, Growth ultrasounds (if indicated) | Screen for gestational diabetes, check for bacteria that could affect newborn, monitor fetal well-being if concerns arise |
Diving Deeper into First and Second Trimester Screening
First-trimester screening: This is performed between 11 and 13+6 weeks. It involves a maternal blood test measuring two substances (PAPP-A and hCG) and a specialized ultrasound called the nuchal translucency (NT) scan. The NT scan measures the clear space at the back of the baby's neck. Together, these results are combined with the mother's age to calculate a risk estimate for Down syndrome and Trisomy 18.
Second-trimester Quad Screen: Offered between 15 and 22 weeks, this blood test measures four substances: AFP, hCG, estriol, and inhibin A. It provides a risk assessment for Down syndrome, Trisomy 18, and open neural tube defects. It is often used for patients who missed first-trimester screening or as part of a sequential screening strategy.
The Anatomy Ultrasound: Typically performed between 18 and 22 weeks, this is a detailed scan recommended for every pregnancy. A sonographer carefully examines the baby's brain, heart, spine, limbs, kidneys, and other organs to check for physical development and any structural abnormalities. It also evaluates the placenta and amniotic fluid levels.
The Role of Ultrasounds and Non-Invasive Prenatal Testing (NIPT/cfDNA)
Ultrasounds are versatile, non-invasive imaging tools used throughout pregnancy. Beyond the NT and anatomy scans, they are used early on to confirm viability and dating, and later to monitor growth and position. Different types include standard 2D, detailed 3D, and real-time 4D imaging.
Non-Invasive Prenatal Testing (NIPT or cell-free DNA screening is a significant advance in prenatal screening. Available from about 10 weeks of pregnancy, it analyzes fragments of the baby's DNA found in the mother's bloodstream. It is highly accurate for screening common chromosomal conditions like Down syndrome, with detection rates over 99% in some studies. It can also reveal the baby's sex.
Professional guidelines now state that cell-free DNA screening can be offered to all pregnant patients as the most sensitive screening option for trisomies 21, 18, and 13. However, it remains a screening test, not a diagnostic one. A positive or high-risk cfDNA result requires follow-up with a diagnostic test like amniocentesis for confirmation.
Navigating Results, Risks, and the Importance of Counseling
Receiving prenatal test results can be an emotional experience. A "screen positive" or high-risk result means the chance for a condition is higher than a set cutoff, not that the baby definitely has it. The next step is typically a discussion with a genetic counselor or maternal-fetal medicine specialist.
Genetic counseling is a key resource. A counselor helps you understand what the results mean, explains the options for further testing, and discusses the potential implications for your pregnancy and baby. They provide support without pressure, helping you make decisions that are right for your family.
When considering diagnostic tests like CVS or amniocentesis, it's important to weigh the small risk of procedure-related pregnancy loss (generally cited as less than 1 in 450 for CVS and less than 1 in 900 for amniocentesis when performed by an expert) against the benefit of obtaining a definitive diagnosis.
Ultimately, the journey through prenatal testing is personal. By understanding the types of tests, their timing, and their purposes, and by utilizing available counseling support, you can make empowered, informed choices for your pregnancy care.
| Test Category | Specific Test Examples | Typical Gestational Timing | Key Purpose & Notes |
|---|---|---|---|
| First-Trimester Screening | Nuchal translucency ultrasound, PAPP-A & hCG blood test | 11 to 13+6 weeks | Early risk assessment for chromosomal conditions; often combined into one result. |
| Second-Trimester Screening | Quad screen (AFP, hCG, estriol, inhibin A) | 15 to 22 weeks | Risk assessment for chromosomal conditions & neural tube defects like spina bifida. |
| Advanced Screening | Cell-free DNA (cfDNA / NIPT) | From 10 weeks onward | Highly accurate screening for common trisomies; screening test, not diagnostic. |
| Imaging | Detailed Anatomy Ultrasound | 18 to 22 weeks | Comprehensive check of fetal structures for physical abnormalities; recommended for all. |
| Diagnostic Procedures | Chorionic Villus Sampling (CVS) | 10 to 14 weeks | Definitive diagnosis of chromosomal conditions; small miscarriage risk. |
| Diagnostic Procedures | Amniocentesis | From 15 weeks onward | Definitive diagnosis of chromosomal conditions & neural tube defects; small miscarriage risk. |
A Guided Journey Through Prenatal Testing: Empowering Your Choices

Introduction to Prenatal Screening and Testing
Prenatal care includes a variety of tests designed to provide information about your baby's health during pregnancy. These tests help you and your healthcare team make informed decisions, prepare for your baby’s arrival, and manage any potential health concerns. The overarching goal is to offer reassurance, early detection, and options for treatment or planning when necessary.
Testing is entirely optional and a personal choice. It involves considering your own values, family history, and medical goals. You have the right to accept or decline any test after discussing the risks and benefits with your doctor or a genetic counselor.
Types of Prenatal Tests: Screening vs. Diagnostic
A fundamental distinction in prenatal testing is between screening tests and diagnostic tests. Understanding this difference is key to making empowered decisions.
Screening tests assess the chance or probability that your baby might have a specific health condition. They are typically non-invasive, involving blood tests and ultrasounds. A screening result might be reported as "low risk" or "increased risk," but it does not provide a definitive diagnosis.
Diagnostic tests, on the other hand, can confirm whether a baby actually has a condition. These procedures, such as chorionic villus sampling (CVS) and amniocentesis, are more invasive and carry a small risk of complications, including miscarriage. They are usually recommended after a high-risk screening result or for individuals with specific risk factors.
| Test Type | Primary Purpose | Common Methods | Key Consideration |
|---|---|---|---|
| Screening | Estimates risk of a condition | Blood tests, ultrasound exams | Results are not definitive; follow-up may be needed |
| Diagnostic | Confirms a diagnosis | Amniocentesis, chorionic villus sampling (CVS) | Invasive; carries a small procedure-related risk |
Understanding the Common Conditions Screened
Prenatal tests focus on a range of genetic conditions and structural birth defects. The most common chromosomal disorders screened for include Down syndrome (trisomy 21), Edwards syndrome (trisomy 18), and Patau syndrome (trisomy 13). Screening also looks for neural tube defects, which affect the brain and spine, such as spina bifida.
Carrier screening is another important category. This involves testing you and your partner, ideally before or early in pregnancy, to see if you carry genes for inherited disorders like cystic fibrosis, spinal muscular atrophy, or sickle cell disease. Knowing your carrier status helps assess the risk to your baby.
Timeline: When Are Tests Typically Offered?
Tests are offered at specific times during pregnancy to ensure accuracy and allow for appropriate follow-up care.
- First Trimester (Weeks 1-13): Initial visits include blood tests to check your health (blood type, infections, immunity) and carrier screening. First-trimester screening for fetal conditions is also offered between 10 and 13 weeks.
- Second Trimester (Weeks 14-27): This period includes second-trimester blood screening (quad screen) and the detailed anatomy ultrasound, typically scheduled between 18 and 22 weeks. Screening for gestational diabetes occurs around 24 to 28 weeks.
- Third Trimester (Week 28 onward): Late-pregnancy care includes a Group B Streptococcus (GBS) culture around 35 to 37 weeks and regular monitoring of fetal well-being.
Diving Deeper into First and Second Trimester Screening
First trimester screening often combines a maternal blood test with a specialized ultrasound called nuchal translucency (NT) screening. The blood test measures specific proteins and hormones. The NT ultrasound measures the clear space at the back of the baby's neck; a larger measurement can be associated with an increased risk for certain conditions.
Second-trimester screening commonly involves the quad screen, a blood test that measures four substances to evaluate risk for chromosomal conditions and neural tube defects. A routine mid-pregnancy ultrasound is also a standard part of care to check the baby’s anatomy and growth.
Some care providers offer combined or sequential screening, which integrates results from tests in both trimesters. This approach can increase the overall detection rate for certain abnormalities.
The Role of Ultrasounds and Non-Invasive Prenatal Testing (NIPT/cfDNA)
Ultrasound is a versatile, non-invasive imaging tool used throughout pregnancy. It helps confirm your due date, check fetal growth, and examine the baby’s anatomy for structural abnormalities. Different types include standard 2D, 3D, and 4D imaging.
Non-Invasive Prenatal Testing (NIPT), also known as cell-free DNA (cfDNA) screening, represents a significant advance in prenatal screening. It is a simple blood test that analyzes small fragments of fetal DNA circulating in the mother's bloodstream.
'What is the most accurate prenatal screening test available?'
Currently, NIPT/cfDNA is considered the most accurate prenatal screening test available for common chromosomal disorders like Down syndrome. Professional guidelines state it has the highest sensitivity and specificity among screening options. For trisomy 21, detection rates are often reported at over 99% with a very low false-positive rate.
It is important to remember that NIPT is a screening test, not a diagnostic one. A result indicating increased risk is not a confirmed diagnosis and should be followed by a diagnostic test like amniocentesis for certainty. NIPT can be performed as early as 10 weeks into pregnancy.
Navigating Results, Risks, and the Importance of Counseling
Receiving and understanding test results is a critical part of the process. Screening tests are not perfect and can sometimes yield false-positive results or false-negative results. A false-positive means the test suggests a higher risk when the baby does not have the condition, which can cause unnecessary anxiety. A false-negative means the test suggests a lower risk but misses an actual condition.
'How accurate are prenatal screening tests in general?'
In general, modern prenatal screening tests are quite accurate for estimating risk, but their performance varies. NIPT has very high accuracy for the conditions it targets. First-trimester combined screening and the second-trimester quad screen are also reliable but have different statistical profiles. The accuracy of any test can be influenced by factors like the specific condition, gestational age, and individual maternal characteristics.
Discussing the detection rates and limitations of each test with your provider is essential. This conversation helps you interpret what a "positive" or "negative" result truly means for your pregnancy.
Genetic counseling is a valuable resource at any stage. A genetic counselor is a healthcare professional with specialized training who can help you understand your test options, interpret complex results, and navigate difficult decisions. Counseling supports informed decision making without pressure, aligning your care with your personal values and circumstances.
| Test Name | Typical Gestational Window | Primary Conditions Screened | Key Consideration |
|---|---|---|---|
| First-Trimester Combined Screen | 10-13 weeks | Down syndrome, trisomy 18 | Combines blood test with NT ultrasound |
| Quad Screen | 15-22 weeks | Down syndrome, trisomy 18, neural tube defects | Second-trimester blood test; not diagnostic |
| NIPT / cfDNA Screening | 10+ weeks | Down syndrome, trisomy 18, trisomy 13, sex chromosome differences | Highest accuracy screening; requires confirmation |
| Anatomy Ultrasound | 18-22 weeks | Structural birth defects | Visual check of fetal anatomy and growth |
| Diagnostic Test (CVS/Amniocentesis) | CVS: 10-14 weeks; Amnio: 15+ weeks | Chromosomal and genetic disorders | Definitive diagnosis; carries procedure risk |
A Guided Journey Through Prenatal Testing: Empowering Your Choices

Introduction to Prenatal Screening and Testing
Prenatal testing provides information about your baby's health during pregnancy. These tests can involve simple blood draws, ultrasounds, or more detailed procedures. The goal is to help you and your healthcare team make informed decisions and prepare for your baby's arrival.
Approximately 3 to 5 percent of pregnancies involve a birth defect or genetic condition. While most babies are born healthy, prenatal genetic testing can identify potential concerns early. Early detection is powerful; it can allow for treatment before birth or help families plan for specialized care immediately after delivery.
Types of Prenatal Tests: Screening vs. Diagnostic
It's essential to understand the two main categories of prenatal genetic tests: screening and diagnostic. They serve very different purposes.
Screening tests estimate the chance or risk that your baby has a specific condition. They are typically non-invasive, involving blood tests and ultrasounds. A "positive" or "high-risk" screening result does not mean your baby has the condition; it means the chance is higher than average and that further diagnostic testing should be considered. Screening tests are not perfect and can have false-positive or false-negative results.
Diagnostic tests, such as chorionic villus sampling (CVS) and amniocentesis, can provide a definitive "yes" or "no" diagnosis for many genetic conditions. These tests analyze fetal cells directly but are invasive and carry a small risk of miscarriage. They are usually offered after a high-risk screening result or for pregnancies with other risk factors.
Understanding the Common Conditions Screened
Prenatal tests primarily screen for chromosomal abnormalities and structural birth defects. The most common chromosomal disorder is Down syndrome (trisomy 21), occurring in about 1 in 800 live births. Other conditions screened for include Edwards syndrome (trisomy 18), Patau syndrome (trisomy 13), and sex chromosome differences.
Screening also looks for neural tube defects, such as spina bifida, which are openings in the spine or brain. Additionally, carrier screening is a separate test for parents that checks if you carry genes for inherited disorders like cystic fibrosis, sickle cell disease, or spinal muscular atrophy.
Timeline: When Are Tests Typically Offered?
Different tests are performed at specific times during pregnancy to ensure accuracy. The following table outlines the typical schedule for key prenatal tests.
| Test Type | Common Name(s) | Typical Gestational Timing | Primary Purpose |
|---|---|---|---|
| Screening | Carrier Screening | Before pregnancy or early 1st trimester | Identify parental gene carriers |
| Screening | First Trimester Combined Screen | 11 to 13 weeks | Assess risk for trisomy 21, 18, and 13 |
| Diagnostic | Chorionic Villus Sampling (CVS) | 10 to 13 weeks | Diagnose chromosomal abnormalities |
| Screening | Quad Screen / Multiple Markers | 15 to 22 weeks | Assess risk for trisomies & neural tube defects |
| Diagnostic | Amniocentesis | 15 to 20 weeks (or later) | Diagnose chromosomal issues & neural tube defects |
| Screening | Cell-free DNA (NIPT) | From 10 weeks onward | Screen for common trisomies & sex chromosomes |
| Screening | Anatomy Ultrasound | 18 to 22 weeks | Check for structural fetal abnormalities |
| Screening | Glucose Challenge Test | 24 to 28 weeks | Screen for gestational diabetes |
| Screening | Group B Strep Culture | 35 to 37 weeks | Check for bacteria to guide labor antibiotics |
Diving Deeper into First and Second Trimester Screening
First-trimester screening usually combines a maternal blood test with a special ultrasound called a nuchal translucency (NT) scan. The blood test measures two pregnancy-associated substances. The NT ultrasound measures the clear space at the back of the baby's neck; a larger measurement can be associated with a higher risk for certain conditions.
Second-trimester screening often involves the "quad screen," a blood test measuring four different markers. This screen provides risk information for Down syndrome, trisomy 18, and open neural tube defects. Combining results from first and second-trimester screenings can improve overall detection rates.
The Role of Ultrasounds and Non-Invasive Prenatal Testing (NIPT/cfDNA)
Ultrasound is a cornerstone of prenatal care. Beyond the NT scan, a detailed anatomy ultrasound around 20 weeks checks the baby's developing organs, limbs, and brain for structural issues. It is a safe, non-invasive imaging tool recommended for every pregnancy.
Non-Invasive Prenatal Testing (NIPT), also called cell-free DNA (cfDNA) screening, is a significant advance. This simple blood test, available from about 10 weeks of pregnancy, analyzes tiny fragments of the baby's DNA circulating in the mother's bloodstream. It is highly accurate for screening for Down syndrome, trisomy 18, and trisomy 13. It can also screen for sex chromosome differences and reveal the baby's sex.
Navigating Results, Risks, and the Importance of Counseling
Understanding test results is crucial. A screening result indicating "high risk" requires follow-up, typically a discussion with a genetic counselor and consideration of diagnostic testing for confirmation. A "low risk" result is reassuring but does not guarantee the baby is unaffected by all conditions.
All tests have considerations. Screening tests can cause anxiety due to false positives. Diagnostic tests like CVS and amniocentesis are very accurate but carry a small procedure-related risk of miscarriage—generally cited as less than 1 in 450 for CVS and less than 1 in 900 for amniocentesis.
This is where genetic counseling becomes invaluable. A genetic counselor is a healthcare professional with specialized training. They do not tell you what to do. Instead, they help you understand the tests, interpret complex results, and explore how the information aligns with your personal values and family goals. Consulting with a counselor or your obstetrician ensures your decisions are fully informed.
What are the ACOG guidelines for prenatal screening and NIPT?
The American College of Obstetricians and Gynecologists (ACOG) states that all pregnant patients should be offered discussion and access to prenatal genetic screening and diagnostic testing, regardless of age or perceived risk. If screening is chosen, patients should select one primary approach. Cell-free DNA (NIPT) is recognized as the most sensitive and specific screening test for common fetal aneuploidies (trisomy 21, 18, and 13) but is not diagnostic. All patients should also be offered a second-trimester ultrasound. Crucially, ACOG emphasizes thorough pre-test counseling, and patients have the right to accept or decline any test after understanding the options.
Is genetic testing recommended differently for pregnancies in individuals over 35?
Yes, recommendations are more proactive for those 35 and older due to the increased risk of chromosomal abnormalities with advanced maternal age. Standard screening options are fully available and often encouraged. Additionally, diagnostic testing like amniocentesis or CVS is discussed in more detail as a direct option due to its definitive nature. The decision remains personal, but comprehensive genetic counseling is strongly advised to navigate the higher statistical risks and the risks and benefits of each test.
| Key Concepts in Prenatal Testing | Purpose / Description | Important Considerations |
|---|---|---|
| Screening Tests | Estimate risk of a condition; non-invasive. | Not diagnostic; can have false results. |
| Diagnostic Tests | Provide a definitive diagnosis; invasive. | Carry small risk of pregnancy loss. |
| Genetic Counseling | Helps interpret results & guide decisions. | Supports informed, personal choice. |
| Cell-free DNA (NIPT) | Highly accurate blood test for screening. | Screens for specific conditions only. |
| Ultrasound | Images fetus to check growth & structure. | Routine part of prenatal care. |
A Guided Journey Through Prenatal Testing: Empowering Your Choices

Introduction to Prenatal Screening and Testing
Prenatal testing is a key part of modern pregnancy care, offering insights into your baby's health during pregnancy before birth. These optional tests provide information that can help you and your healthcare team make informed decisions. They are broadly divided into two categories: screening tests and diagnostic tests. Their primary goal is to identify the risk or presence of certain genetic conditions and birth defects. This allows for advanced planning, potential treatment during pregnancy, or preparation for specialized care after delivery.
About 3 to 5 percent of pregnancies are affected by a birth defect or genetic disorder. While this means most babies are born healthy, prenatal testing offers a way to understand your specific pregnancy better. It's a personal choice, influenced by your values, family history, and health goals. Consulting with your doctor or a genetic counselor is the best first step to navigate these options.
Types of Prenatal Tests: Screening vs. Diagnostic
Understanding the fundamental difference between screening and diagnostic tests is crucial.
Screening tests estimate the chance or risk that a baby might have a specific condition. They do not provide a definitive 'yes' or 'no' answer. These are generally non-invasive and safe, involving procedures like blood draws and ultrasounds. Common examples include first-trimester screening, the quad screen, and Non-Invasive Prenatal Testing (NIPT).
Diagnostic tests, such as chorionic villus sampling (CVS) and amniocentesis, can provide a conclusive diagnosis. They involve collecting fetal or placental cells to analyze chromosomes directly. Because they are invasive procedures, they carry a small risk of complications, including miscarriage. These tests are typically offered after a high-risk screening result or due to other risk factors.
| Test Type | Purpose | Method | Key Consideration |
|---|---|---|---|
| Screening | Assesses risk or probability | Blood test, ultrasound | Results are not definitive |
| Diagnostic | Confirms a specific condition | CVS, amniocentesis | Carries a small procedural risk |
Understanding the Common Conditions Screened
Prenatal tests focus on identifying risks for specific categories of health conditions. Knowing what is being looked for can help you understand your results.
Chromosomal Abnormalities: These involve extra or missing chromosomes. The most common is Down syndrome (trisomy 21). Other screened conditions include trisomy 18 (Edwards syndrome) and trisomy 13 (Patau syndrome). The risk for these conditions increases with maternal age.
Neural Tube Defects (NTDs): These are birth defects of the brain and spine, such as spina bifida. Screening for NTDs is typically done in the second trimester by measuring a protein called alpha-fetoprotein (AFP) in the mother's blood.
Inherited Genetic Disorders: Carrier screening is a separate type of test performed on parents, ideally before or early in pregnancy. It checks if you carry a gene for conditions like cystic fibrosis, sickle cell disease, or spinal muscular atrophy, which could be passed to your baby.
Timeline: When Are Tests Typically Offered?
Prenatal tests are offered at specific times during pregnancy to ensure accuracy. The following table outlines a general schedule.
| Trimester | Weeks Gestation | Common Tests Offered | Primary Focus |
|---|---|---|---|
| First | 10-13 weeks | First-trimester combined screen, CVS, NIPT | Early risk assessment for chromosomal issues |
| Second | 15-22 weeks | Quad screen, anatomy ultrasound, amniocentesis | Broader screening for chromosomes & NTDs |
| Late Second/Third | 24-28 weeks | Glucose challenge test | Screening for gestational diabetes |
| Late Third | 35-37 weeks | Group B Streptococcus (GBS) culture | Checking for bacteria that can affect newborn |
Diving Deeper into First and Second Trimester Screening
First-Trimester Screening is often a combined test performed between weeks 10 and 13. It includes a maternal blood test measuring two pregnancy hormones and a special ultrasound called a nuchal translucency (NT) scan. The NT scan measures the clear space at the back of the baby's neck. Together, these results estimate the risk for Down syndrome and trisomy 18.
Second-Trimester Screening usually involves the "quad screen" blood test (measuring four substances) between 15 and 22 weeks. It assesses risk for the same chromosomal conditions and also screens for open neural tube defects. A detailed anatomy ultrasound around 18-22 weeks is also a standard part of second-trimester care, checking for physical development and structural abnormalities.
Some care providers offer integrated or sequential screening, which combines results from tests in both trimesters for a single, more accurate risk assessment.
The Role of Ultrasounds and Non-Invasive Prenatal Testing (NIPT/cfDNA)
Ultrasound is a versatile, non-invasive imaging tool used throughout pregnancy. In the first trimester, it helps establish an accurate due date. The mid-pregnancy anatomy scan provides a detailed check of fetal growth and organ development. Advanced 3D and 4D ultrasounds can offer more detailed views but are not routinely required for medical diagnosis.
Non-Invasive Prenatal Testing (NIPT), also called cell-free DNA (cfDNA) screening, is a significant advance. This is a blood test that analyzes tiny fragments of the baby's DNA circulating in the mother's bloodstream. It can be done as early as 10 weeks and is highly accurate for screening common trisomies like Down syndrome. It can also reveal the baby's sex. However, it is important to remember NIPT is still a screening test, not a diagnostic one, and positive results require confirmation.
Navigating Results, Risks, and the Importance of Counseling
Receiving and understanding test results is a critical phase. A screening test will report your results as a risk level—either "screen positive" (higher risk) or "screen negative" (lower risk). A screen positive does not mean your baby has the condition; it means you should discuss follow-up options, which usually include diagnostic testing for confirmation.
All tests have limitations. Screening tests can produce false-positive results (indicating a risk when none exists) or false-negative results (missing an actual risk). Diagnostic tests like CVS and amniocentesis are very accurate but carry a small risk of pregnancy loss, estimated at less than 1 in 450 for CVS and less than 1 in 900 for amniocentesis when performed by an experienced specialist.
What are the pros and cons of prenatal screening tests?
Prenatal screening tests offer several significant benefits. The primary advantage is providing expectant parents with valuable, early information about their baby's risk for certain genetic conditions, such as Down syndrome, which allows for better prenatal care planning and emotional preparation. These tests are non-invasive, typically involving only a blood draw and an ultrasound, posing no physical risk to the pregnancy.
However, there are important considerations. Screening tests are not diagnostic; they only assess risk, which can sometimes lead to false-positive results causing unnecessary anxiety. Conversely, false-negative results can provide false reassurance. Furthermore, an abnormal screening result presents parents with a difficult decision about whether to pursue invasive diagnostic testing, such as amniocentesis, which carries a small risk of miscarriage. Ultimately, these screenings are optional, and the choice involves weighing the desire for information against the potential for uncertain results and subsequent difficult decisions.
This underscores the vital role of genetic counseling. A genetic counselor is a trained professional who can help you understand the different tests, their accuracy, potential risks, and what the results mean for your family. They provide support without pressure, ensuring your decisions align with your personal values and healthcare goals. Professional guidelines recommend that all patients receive this counseling before making decisions about prenatal testing.
| Topic Category | Specific Tests & Procedures | Key Patient Consideration |
|---|---|---|
| Early Screening | First-trimester screen, NT ultrasound | Provides an early risk estimate |
| Mid-Pregnancy Screening | Quad screen, anatomy scan | Screens for chromosomes & physical defects |
| Advanced Screening | NIPT / cfDNA | High accuracy for common trisomies |
| Diagnostic Procedures | CVS, amniocentesis | Provides a definitive diagnosis |
| Support & Decision-Making | Genetic counseling, doctor consultation | Essential for understanding options & results |
A Guided Journey Through Prenatal Testing: Empowering Your Choices

Introduction to Prenatal Screening and Testing
Prenatal testing provides valuable information about a baby's health during pregnancy. It helps parents understand potential genetic conditions or birth defects. This knowledge enables informed decisions about pregnancy management and future care plans. These tests are a standard part of prenatal care offered to all pregnant individuals. However, it is important to remember that prenatal genetic testing is optional. The choice to undergo prenatal testing is a personal one, guided by individual values and healthcare goals. Consulting with a healthcare professional is the first step on this journey.
Types of Prenatal Tests: Screening vs. Diagnostic
Understanding the two main categories of prenatal tests is crucial for making informed choices.
Screening Tests: These tests assess the risk or likelihood that a baby might have certain conditions. They cannot provide a definitive diagnosis. Screening methods typically involve blood tests and ultrasounds. Results are often reported as a probability, such as a "higher risk" or "lower risk" finding. They are generally non-invasive and carry no risk to the pregnancy.
Diagnostic Tests: These are the only tests that can confirm, or rule out, a specific genetic condition. Procedures like chorionic villus sampling (CVS) and amniocentesis fall into this category. Because they involve obtaining fetal or placental cells, they carry a small risk of miscarriage. Diagnostic testing is usually recommended after a high-risk screening result or due to factors like advanced maternal age or family history.
| Test Type | Primary Purpose | Common Procedures | Key Risk Consideration |
|---|---|---|---|
| Screening | Estimates probability of a condition | Blood tests, ultrasounds, NIPT/cfDNA | None to pregnancy; potential for false results |
| Diagnostic | Provides definitive yes/no diagnosis | Amniocentesis, chorionic villus sampling (CVS) | Small risk of miscarriage |
What conditions or diseases can be detected through genetic testing during pregnancy?
Genetic testing during pregnancy can identify a broad spectrum of conditions. Screening tests, such as cell-free DNA (cfDNA) analysis, assess the risk for common chromosomal abnormalities. These include Down syndrome (trisomy 21), Edwards syndrome (trisomy 18), and Patau syndrome (trisomy 13).
They can also screen for sex chromosome differences like Turner syndrome and Klinefelter syndrome. Diagnostic tests like amniocentesis can confirm these conditions and test for specific inherited disorders. This includes cystic fibrosis, sickle cell disease, Tay-Sachs, or spinal muscular atrophy when indicated by family history. Importantly, prenatal ultrasounds and a blood test measuring maternal serum alpha-fetoprotein (AFP) are key for detecting structural issues like open neural tube defects, including spina bifida.
Timeline: When Are Tests Typically Offered?
Testing follows a schedule aligned with pregnancy trimesters. This timeline allows for appropriate risk assessment and decision-making at different stages.
- First Trimester (Weeks 1-13): Initial prenatal visits include blood tests to check the mother's health. First-trimester screening for fetal conditions is typically offered between 10 and 13 weeks. This often combines a blood test with a nuchal translucency ultrasound.
- Second Trimester (Weeks 14-26): The quad screen blood test is offered between 15 and 22 weeks. A detailed routine anatomy ultrasound is recommended for every pregnancy, ideally between 18 and 22 weeks.
- Throughout Pregnancy: Some tests, like prenatal cell-free DNA screening, can be performed after 10 weeks in any trimester. Later in pregnancy, routine screenings for gestational diabetes (24-28 weeks) and Group B Streptococcus (35-37 weeks) are standard.
Diving Deeper into First and Second Trimester Screening
First Trimester Screening usually combines two components. A maternal blood test measures specific proteins and hormones. A nuchal translucency ultrasound measures the clear space at the back of the baby's neck. An increased measurement can indicate a higher risk for chromosomal conditions or certain heart defects.
Second Trimester Screening often involves the "quad screen." This blood test measures four substances to evaluate risk for chromosomal conditions and neural tube defects. Abnormal levels of alpha-fetoprotein (AFP), one of these markers, may prompt further investigation with a detailed ultrasound.
Many healthcare providers also offer combined or sequential screening. This integrates results from both the first and second trimester tests. This approach can increase the overall detection rate for certain conditions like Down syndrome.
The Role of Ultrasounds and Non-Invasive Prenatal Testing (NIPT/cfDNA)
Pregnancy ultrasound is a versatile, non-invasive imaging tool used throughout pregnancy. In the first trimester, it helps establish an accurate due date. The mid-pregnancy anatomy scan provides a detailed check of fetal development and structure. Different types, including 3-D and 4-D imaging, offer various levels of detail. Ultrasound is considered very safe, using sound waves instead of radiation.
Cell-Free DNA (cfDNA) Screening, often called NIPT or NIPS, is a significant advance in prenatal screening. This is a blood test that analyzes fetal DNA circulating in the mother's bloodstream. It screens for specific chromosomal conditions with high accuracy, particularly for Down syndrome. It can also reveal the baby's sex. ACOG and other societies note it is the most sensitive and specific screening test for common fetal aneuploidies. It is important to know it is still a screening test, not a diagnostic one.
Navigating Results, Risks, and the Importance of Counseling
Understanding test results is a critical part of the process. A "positive" or "high-risk" screening result does not mean the baby definitely has a condition. It indicates an increased probability, and follow-up diagnostic testing is offered for confirmation. Conversely, a "negative" or "low-risk" result significantly reduces the likelihood but does not guarantee the baby is unaffected.
All tests have limitations. Screening tests can produce false-positive results or false-negative results. Diagnostic tests, while definitive, carry a small procedure-related risk. This is why genetic counseling is so valuable. A genetic counselor is a specialized healthcare professional who can help you:
- Understand your personal risk factors.
- Interpret screening and diagnostic test results.
- Weigh the risks and benefits of different testing options.
- Plan for next steps based on your family's values and goals.
Meeting with a counselor provides support and clarity, empowering you to make the choices that are right for your pregnancy journey.
Topics Covered in This Section
| Main Topic Area | Specific Details Covered | Key Takeaway for Patients |
|---|---|---|
| Test Categories | Screening vs. diagnostic purposes | Screening estimates risk; diagnostic provides a yes/no answer. |
| Conditions Detected | Chromosomal issues & inherited disorders | Tests can assess risk for Down syndrome, spina bifida, cystic fibrosis, and more. |
| Testing Timeline | First & second trimester options | Specific tests are offered at different points in pregnancy. |
| Common Procedures | Ultrasounds, blood tests, NIPT, CVS, amniocentesis | Each test has a specific role, accuracy, and risk profile. |
| Result Interpretation | Understanding positive/negative screening test results explained | A high-risk screening result requires diagnostic testing for confirmation. |
| Support Resources | Role of genetic counseling & healthcare providers | Counseling helps navigate complex information and personal choices. |
A Guided Journey Through Prenatal Testing: Empowering Your Choices
Introduction to Prenatal Screening and Testing
Prenatal testing is a cornerstone of modern pregnancy care. It provides valuable information about your baby's developing health, offering insights into potential genetic conditions or birth defects. The primary goal is to empower expectant parents with knowledge. This knowledge enables informed decision-making about pregnancy management and future care for their child. It's important to remember that while prenatal testing is recommended for all pregnant patients, it is always optional. Making an informed choice that aligns with your personal values and healthcare goals is a crucial first step on this journey.
Types of Prenatal Tests: Screening vs. Diagnostic
Understanding the fundamental difference between screening and diagnostic tests is key. These two types serve distinct purposes in your prenatal care. Screening tests assess the risk or likelihood that a baby might have certain genetic conditions. They are typically non-invasive, involving blood draws or ultrasounds. However, they cannot provide a definitive diagnosis. An abnormal screening result indicates a higher chance and prompts further investigation. Diagnostic tests, such as chorionic villus sampling (CVS) and amniocentesis, are the only way to definitively confirm if a baby has a genetic condition. These procedures are more invasive and carry a slight risk of pregnancy loss. They are usually recommended after a high-risk screening result or for women with specific risk factors.
Understanding the Common Conditions Screened
Prenatal tests are designed to screen for or diagnose specific conditions. Chromosomal aneuploidies, where a fetus has missing or extra chromosomes, are a primary focus. The most common is Down syndrome (trisomy 21), occurring in about 1 in 800 live births. Tests also screen for Edwards syndrome (trisomy 18) and Patau syndrome (trisomy 13). Another major category is neural tube defects (NTDs), such as spina bifida and anencephaly, which affect the developing brain and spine. Genetic disorders like cystic fibrosis, sickle cell disease, and spinal muscular atrophy can be assessed through carrier screening, which tests prospective parents to see if they carry a gene for an inherited condition.
| Condition Category | Specific Examples | Key Fact |
|---|---|---|
| Chromosomal Aneuploidy | Down syndrome (Trisomy 21), Edwards syndrome (Trisomy 18), Patau syndrome (Trisomy 13) | Risk increases with maternal age. |
| Neural Tube Defects (NTDs) | Spina bifida, Anencephaly | Screened via a protein called Alpha-fetoprotein (AFP). |
| Inherited Genetic Disorders | Cystic fibrosis, Sickle cell disease, Spinal muscular atrophy | Carrier screening is often recommended for parents. |
Timeline: When Are Tests Typically Offered?
Prenatal testing follows a schedule aligned with pregnancy trimesters and fetal development. Carrier screening can be done before or during pregnancy. First-trimester screening is typically offered between 10 and 13 weeks. Second-trimester screening usually occurs between 15 and 22 weeks. Diagnostic tests also have specific windows: CVS is performed between 10 and 13 weeks, while amniocentesis is done after 15 weeks. Non-invasive prenatal testing (NIPT/cfDNA) can be done starting at 10 weeks. Later in pregnancy, screenings for gestational diabetes (24-28 weeks) and Group B Strep (35-37 weeks) are standard. Your provider will guide you through this timeline.
Diving Deeper into First and Second Trimester Screening
The first and second trimesters offer specific screening combinations. First-trimester screening often includes a maternal blood test (measuring PAPP-A and hCG) and a special ultrasound called nuchal translucency (NT). The NT measures the clear space at the back of the baby's neck; a larger measurement can be associated with an increased risk for certain conditions. Second-trimester screening often involves the quad screen, a blood test measuring four substances (AFP, hCG, estriol, and inhibin A) to assess risk for chromosomal conditions and NTDs. A routine anatomy ultrasound, recommended for every pregnancy around 18-22 weeks, thoroughly checks the baby's physical structure. Some practices use combined or sequential screening strategies that integrate results from both trimesters for higher accuracy.
The Role of Ultrasounds and Non-Invasive Prenatal Testing (NIPT/cfDNA)
Ultrasound is a versatile, non-invasive imaging tool used throughout pregnancy. In the first trimester, it confirms the due date and checks for early viability. The mid-pregnancy anatomy scan provides a detailed look at fetal organs and limbs. Non-Invasive Prenatal Testing (NIPT), also called cell-free DNA (cfDNA) screening, is a significant advancement. It analyzes tiny fragments of fetal DNA circulating in the mother's blood, starting as early as 10 weeks. For common trisomies like Down syndrome, NIPT has a very high detection rate (over 99%) and a low false-positive rate. It can also screen for some sex chromosome differences and, in many cases, reveal the baby's sex. It's important to know that NIPT is a screening test, not a diagnostic one, and a positive result requires follow-up with a diagnostic procedure for confirmation.
Navigating Results, Risks, and the Importance of Counseling
Receiving and interpreting test results is a critical phase. A positive screening result means your baby has a higher risk for a condition compared to the general population—it is not a diagnosis. A negative result indicates a lower risk but does not guarantee the baby is unaffected. All screening tests have a potential for false-positive and false-negative results, which can cause anxiety. Diagnostic tests like CVS and amniocentesis carry a small but real risk of procedure-related pregnancy loss, estimated at less than 1 in 450 for CVS and less than 1 in 900 for amniocentesis. This is why genetic counseling is invaluable. A genetic counselor is a specialized healthcare professional who can help you understand the risks, benefits, and limitations of each test, interpret complex results, and support you in making decisions that are right for your family. Consulting with your obstetrician or a genetic counselor ensures your journey through prenatal testing is informed, thoughtful, and tailored to your unique situation.
| Test Type | Common Examples | Primary Purpose | Key Consideration |
|---|---|---|---|
| Screening | First-trimester screen, Quad screen, NIPT/cfDNA | Assess risk or likelihood of a condition. | Not diagnostic; can have false results. |
| Diagnostic | Chorionic Villus Sampling (CVS), Amniocentesis | Provide a definitive diagnosis. | Invasive; carries a small miscarriage risk. |
| Imaging | Nuchal Translucency (NT) ultrasound, Anatomy scan | Visualize fetal growth and structure. | Non-invasive; no known radiation risk. |
| Parental Screen | Carrier screening (cystic fibrosis, etc.) | Determine if parents carry genes for inherited disorders. | Informs family planning and fetal risk. |





.png)