The Truth About Birth Control Pills: What Medical Experts Want You to Know

Why Pelvic Floor Health Matters for VBAC
VBAC attempts succeed in 60‑80 % of low‑risk pregnancies, with a uterine‑rupture risk of about 1 in 300. A well‑conditioned pelvic floor supports the uterus, bladder and perineum, helping to control intra‑abdominal pressure, reduce perineal tearing and improve pushing efficiency. Strengthening these muscles also lowers the chance of postpartum incontinence and speeds recovery after birth. Preparation combines three pillars: (1) regular, pregnancy‑safe aerobic activity such as walking or swimming; (2) targeted pelvic‑floor training – Kegels, diaphragmatic breathing, deep squats and cat‑cow stretches – performed several times daily; and (3) professional support, including a pelvic‑health physical therapist, a VBAC‑friendly obstetrician and a doula. Together they enhance mobility, scar tissue flexibility and optimal labor positioning, giving the baby the best chance for a safe vaginal birth.
Pelvic Floor Exercise Fundamentals for VBAC
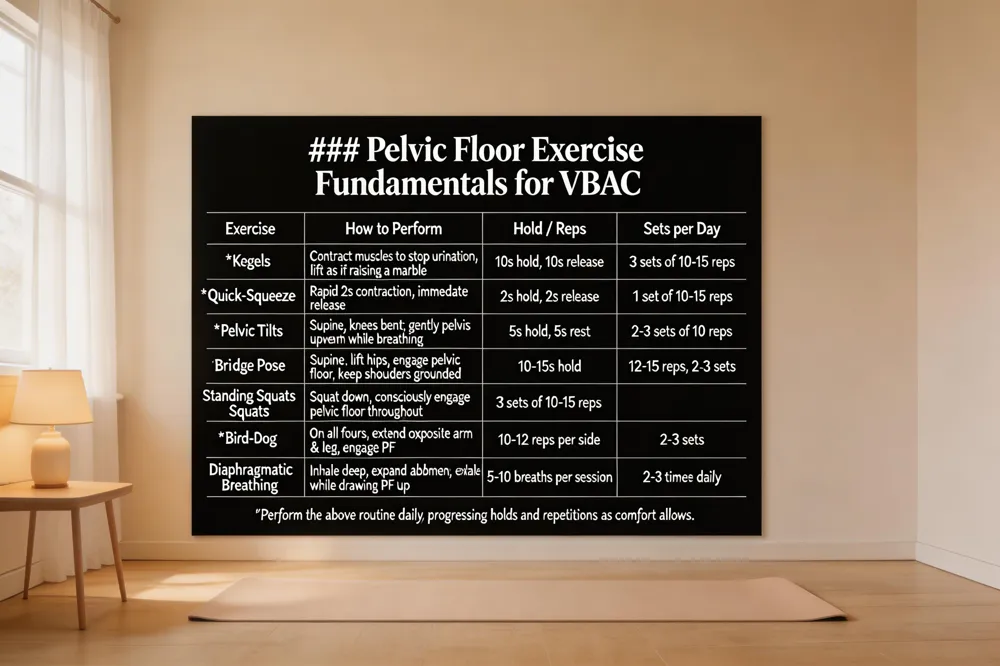 A strong, flexible pelvic floor is a cornerstone of VBAC preparation.
Pelvic floor exercises for VBAC – Kegels strengthen the muscles that support the uterus, bladder and and rectum, making pushing easier and reducing incontinence. To perform a Kegel, contract the muscles you would use to stop urinating, hold for about ten seconds, then release; repeat 10‑15 times, three sets daily. Add core‑stability moves such as pelvic tilts and diaphragmatic breathing (inhale deep, expand the abdomen; exhale while gently drawing the pelvic floor up) to improve coordination and lower intra‑abdominal pressure.
Kegel exercises for women – Locate the correct muscles by stopping the urine stream, then lift as if raising a marble for 3‑6 seconds, relax for the same count. Practice in lying, seated, and standing positions, aiming for three sets of 10‑15 repetitions each day.
Pelvic floor exercises step by step – Begin with isolated squeezes (5‑second hold, 5‑second rest), then bridge pose (lift hips, engage pelvic floor, hold 10‑15 seconds, 12‑15 reps), standing squats with pelvic floor activation (3 sets of 10‑15), and bird‑dog on all fours (10‑12 reps each side).
How to tighten pelvic floor muscles quickly – Use rapid “quick‑squeeze” contractions (2‑second hold, relax) for 10‑15 reps, followed by sustained squeezes (5‑10 seconds). Complement with bridges, squats, and bird‑dog to reinforce core and glute support.
Can pelvic floor exercises help a VBAC? – Yes. Pelvic floor physical therapy educates on anatomy, provides tailored strengthening, and teaches optimal labor positioning, all of which increase the likelihood of a successful VBAC.
Preparing After Multiple Cesareans
 Women who have had two prior C‑sections can still be VBAC candidates when both incisions are low‑transverse scars, the uterine scar has healed, and the inter‑pregnancy interval is at least 18‑24 months. A supportive birth team—ob‑ianian, midwife, or doula experienced with trial‑of‑labor after cesarean—helps coordinate continuous fetal monitoring, rapid surgical backup, and individualized labor positioning.
How to prepare for VBAC after two C‑sections – Confirm low‑transverse scars, allow adequate scar healing time, and choose a provider who advocates for VBAC. Strengthen hips, spine, and pelvic floor through PT‑guided exercises (diaphragmatic breathing, deep squats, cat‑cow stretches) and maintain a balanced, high‑fiber diet with proper hydration. Attend VBAC classes, use a doula, and plan for a hospital equipped for emergency C‑section.
How to prepare for a natural birth after a C‑section – Schedule a thorough OB‑GYN evaluation, engage in pregnancy‑safe core and pelvic‑floor work, stay active with walking or prenatal yoga, and create a birth plan that outlines monitoring preferences and support.
Tips for a normal delivery after a cesarean – Early confirmation of low‑transverse scar, healthy weight, regular low‑impact exercise and a VBAC‑focused birth class improve labor progress while minimizing unnecessary interventions.
VBAC calculator – An online tool that combines age, BMI, prior vaginal births, and indication for the previous C‑section to estimate success probability; it aids counseling but does not replace personalized clinical assessment.
VBAC diet and exercise (general) – Emphasize whole‑food meals rich in fiber, lean protein, and healthy fats; stay well‑hydrated; avoid heartburn‑triggering foods; and practice daily low‑impact cardio, pelvic‑floor Kegels, and gentle stretches to build endurance for labor.
Post‑C‑section Pelvic Floor Recovery
 After a C‑section, gentle activation of the diaphragm and pelvic floor can begin as soon as the incision is stable, usually within the first week. Short walks, deep‑breathing, and light “drawing‑in” abdominal breaths engage core muscles without stressing the scar. Scar‑mobility work—soft massage, gentle heel‑slides, and pelvic‑tilt drills—helps restore tissue glide once cleared by your provider (typically 4‑6 weeks postpartum). Pelvic floor physical therapy starts at 6‑8 weeks, focusing first on diaphragmatic breathing, relaxed Kegel‑style pulls, and cat‑cow stretches; progression moves to coordinated heel‑slides, bridges, and longer holds as pain subsides. Women two weeks postpartum may start diaphragmatic breathing and light Keggs while nursing or walking, aiming for a few seconds per squeeze and 8‑10 repetitions. Strengthening later includes 2‑3 daily sets of slow Keggs (2‑3 seconds hold) and longer 5‑10 second holds, always keeping the abdomen relaxed. A tight pelvic floor after surgery is common; gentle scar‑mobility, breathing, and therapist‑guided stretching relieve tension, improve core stability, and prepare the body for activities or a VBAC.
Resources, Classes, and Support

VBAC classes near me
If you’re looking for VBAC (Vaginal Birth After Cesarean) classes near Queens, NY, start by checking with local obstetrics and gynecology practices such as Raveco, which often offer group workshops or one‑on‑one counseling on VBAC preparation. Queens hospitals—including NewYork‑Presbyterian/Queens, Mount Sinai Queens, and Queens Hospital Center—run scheduled VBAC education sessions covering labor safety, pain‑management techniques, and decision‑making strategies. Community health centers and doula organizations frequently host free or low‑cost VBAC classes, sometimes in partnership with certified nurse‑midwives. Virtual VBAC courses are also available from reputable providers. Call your provider’s office or visit their website to confirm dates, registration requirements, and any fees.
Postpartum pelvic floor exercises PDF
Download our free “Postpartum Pelvic Floor Exercise” PDF, a step‑by‑step guide created by our women‑led obstetrics team in Queens, NY. It outlines safe Kegel routines, breathing tips, progress‑tracking charts, and modifications for diastasis recti. All exercises are illustrated with clear visuals, making it easy to practice at home while caring for your newborn. Click here to download and begin your personalized recovery plan today.
Pelvic floor exercises PDF with pictures
Yes—our clinic offers a printable PDF with illustrated pelvic‑floor exercises such as bridges, clamshells, and seated contractions. Download it from the “Resources” page; the file opens in a new tab for you to save or print. If you have questions, schedule a consultation with a pelvic‑floor physical therapist.
VBAC calculator
An online VBAC calculator estimates the probability of a successful vaginal birth after a prior cesarean by factoring age, BMI, obstetric history, and the indication for the previous C‑section. It uses regression models from large cohort studies to generate a personalized success rate, aiding counseling and shared decision‑making. At our Queens practice we incorporate this tool into comprehensive prenatal care, but it does not replace an individualized clinical assessment by your obstetrician.
Pelvic floor exercises before and after pregnancy
Begin early in pregnancy by locating the pelvic floor (stop urine flow) and performing 5‑10‑second Kegel squeezes, 10‑15 repetitions, three times daily. Add low‑impact core moves—bridge poses, pelvic tilts, bird‑dog extensions—as you progress. After delivery, start with gentle Kegels and short squeezes, gradually increasing hold times and adding squats and bridges once cleared by your provider. Aim for three sets of 10 long squeezes and 10 short squeezes each day, with core exercises 2‑3 times weekly. Consistent practice before and after pregnancy helps prevent incontinence, prolapse, and supports a smoother postpartum recovery.
Putting It All Together: A VBAC Success Plan
 A successful VBAC starts with a clear weekly exercise schedule, balanced nutrition, strategic labor positioning, and a coordinated birth team. • Exercise: Aim for 150‑200 minutes of low‑impact activity each week—walking, swimming, prenatal yoga, and light resistance work. Include daily pelvic‑floor training (Kegels 8‑10 s hold × 10‑15 reps × 3 sets) and a short “quick‑flash” set for fast‑twitch fibers. Add hip‑openers, cat‑cow, and deep‑squat stretches 2‑3 times weekly to improve mobility and scar tissue glide. • Nutrition & Hydration: Follow a whole‑food diet rich in fiber, lean protein, iron, omega‑3s, and plenty of water (2‑3 L/day). Limit added sugars and heartburn‑triggering foods; this supports energy, bowel regularity, and scar healing. • Labor Positioning & Breathing: Practice Diaphragmatic breathing—inhale through the nose to expand the belly, exhale slowly through the mouth—to keep the pelvic floor relaxed and reduce intra‑abdominal pressure. Rehearse upright positions (walking, standing, stability‑ball squat) that open the pelvis and aid fetal descent. • Birth Team Coordination: Choose a supportive obstetrician or midwife, engage a VBAC‑experienced doula, and discuss a birth‑plan that includes early mobility, pain‑management options, and emergency C‑section protocols. Early education and a trusted team lower intervention rates and improve confidence for a safe, successful VBAC.
Your Path to a Strong Pelvic Floor and a Confident VBAC
Preparing for a VBAC begins with consistent pelvic‑floor training, cardio, and flexibility work. Kegels (3‑5 second holds, 10‑15 repetitions, 2‑3 sets), diaphragmatic breathing, deep‑squat stretches, and cat‑cow mobilizations improve strength, coordination, and pelvic opening. Scar‑mobilization and hip‑hinge drills reduce tension on the uterine scar and promote better alignment. Professional support is essential: a pelvic‑health physical therapist can tailor exercises, assess scar mobility, and teach pushing techniques; a VBAC‑experienced doula offers emotional and practical assistance; and a supportive obstetrician or midwife ensures care. For patients in Queens, New York, clinics such as Foundations Pelvic Health or local VBAC‑friendly hospitals provide PT appointments, doula referrals, and prenatal classes. Schedule a consultation early in the second trimester to build strength and confidence before labor. This plan empowers you to achieve a positive safe birth experience.





.png)